Seborrheic Keratoses and Removal- Dermatology
What is seborrheic keratosis?
Seborrheic keratosis is a common benign skin tumor. It is usually prevalent throughout middle age and older-age and rarely during younger age. Seborrheic keratoses are not precancerous. They are one of the most common types of skin growths observed by primary care physicians and dermatologists during routine clinic visits.
They are usually raised above the skin and one can feel them even if they are flat. As seborrheic keratoses are benign, treatment is usually not required. Nevertheless, most patients prefer to undergo some type of treatment. As they are highly prevalent, it is imperative to understand available treatment options for the management of seborrheic keratosis.
Etiology:
Seborrheic keratoses are caused by the benign proliferation of immature keratinocytes, which results in round or oval, flat-shaped macules. In the beginning they are thin in size but their thickness increases over time.
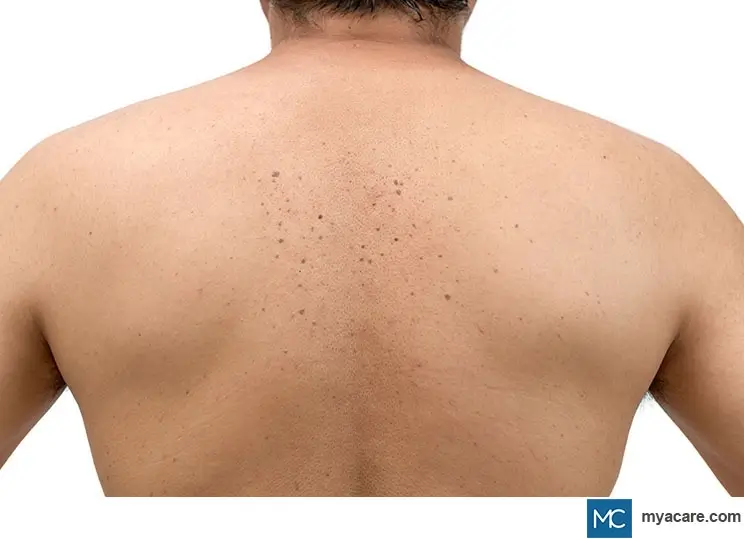
Seborrheic keratoses are not contagious and they are not viral or bacterial. They commonly occur in adults over 50, and tend to multiply during older age. Sun exposure might augment the occurrence of seborrheic keratosis. People with family history of seborrheic keratoses may have a higher chance of developing them. People with light-colored skin are also at risk of getting seborrheic keratoses. Seborrheic keratoses may develop during pregnancy or following an estrogen replacement therapy. The number of seborrheic keratoses usually augments with age.
Children rarely develop seborrheic keratoses.
Symptoms:
Following are the symptoms of seborrheic keratosis:
- Itching but no pain at the site of seborrheic keratosis
- Irritation from friction
- In the beginning they appear as small, rough bumps, then slowly thicken and develop a warty surface
- They have a waxy, stuck-on-the-skin appearance.
- They are generally brown in color, but can also appear black or tan, and in rare instances can be pink, yellow or white.
- They range in size from a fraction of an inch to larger than a half-dollar
- They may appear on the face, chest, back, stomach, scalp, neck, or other parts of the body. However, they do not appear on the palms and soles.
Diagnosis:
The first step in diagnosis of seborrheic keratosis is examination. A dermatologist or primary care physician can recognize the skin growth if it is a seborrheic keratosis by observation with naked eye. If seborrheic keratoses appear as a skin cancer, the dermatologist may suggest removing it for further investigation, which is done under a microscope. This would help to understand if the growth is skin cancer or not.
Treatment:
Seborrheic keratoses are benign and usually do not require any treatment. Due to cosmetic reasons, most of the patients prefer some sort of treatment. Various treatment options are available for the removal of seborrheic keratoses. The dermatologist may recommend biopsy of the lesion if there is bleeding and rapid growth after removing it. Treatment is decided based on the size and thickness of the lesion, skin type, family history, clinical suspicion for malignancy, and the dermatologist’s clinical observation and experience.
The dermatologist or primary care physician can remove seborrheic keratosis using one of the following techniques:
- Cryotherapy: Cryotherapy is the most common and readily available treatment option. Treatment with cryotherapy is effective and usually well tolerated by the patient. The dermatologist or primary care physician will first numb the skin and then use liquid nitrogen to freeze the skin growth, which results in cell death. After the treatment, the skin growth usually falls off within a few days or weeks. Cryotherapy is usually preferred when there is no suspicion of malignancy and no need to preserve a sample of the growth for additional tests or biopsy. It also has a low post-procedure care requirement for the treated area. There may be some pain at the treated area after the treatment. One possible side effect includes lighter skin at the spot from where skin growth was removed.
- Electrodessication/Curettage: The dermatologist or primary care physician will numb the skin and then use a targeted electrocurrent to burn the seborrheic keratosis. A surgical device called a curette is used to scrape away the remains of skin growth. In some instances, electrodessication and curettage are used individually. The risk of scarring is usually low with both techniques. However, following the procedure, patient would be required to take care of the wound till it heals properly.
- Shave excision: This technique is preferred when there is a need to preserve a sample of skin growth for further analysis in the laboratory. After numbing the skin, the dermatologist will cautiously shave off the growth and smooth the skin underneath with a surgical curette. The shaved growth would be further analyzed in the laboratory.
- Laser therapy: Lasers therapy is an alternative option to surgery. During the treatment with laser, the growth is burnt and the wound is sterilized and tissue is sealed at once. Although this technique is quick, the wound would be sore for a while afterward. Laser therapy is associated with good cosmetic outcomes.
- Prescription Hydrogen Peroxide: A topical solution of 40% hydrogen peroxide, through an applicator pen, is applied to seborrheic keratosis numerous times during a single visit to the clinic. Patients may require more than one visit to the clinic based on the severity of seborrheic keratosis. The common side effect includes mild skin reactions.
References:
- Greco MJ, Bhutta BS. Seborrheic Keratosis. [Updated 2022 Feb 9]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK545285/
- Seborrheic Keratosis. Available at: https://my.clevelandclinic.org/health/diseases/21721-seborrheic-keratosis
- Seborrheic keratoses: signs and symptoms. Available at: https://www.aad.org/public/diseases/a-z/seborrheic-keratoses-symptoms
- Seborrheic keratoses: who gets and causes. Available at: https://www.aad.org/public/diseases/a-z/seborrheic-keratoses-causes
- Seborrheic keratoses: diagnosis and treatment. Available at: https://www.aad.org/public/diseases/a-z/seborrheic-keratoses-treatment
Disclaimer: Please note that Mya Care does not provide medical advice, diagnosis, or treatment. The information provided is not intended to replace the care or advice of a qualified health care professional. The views expressed are personal views of the author and do not necessarily reflect the opinion of Mya Care. Always consult your doctor for all diagnoses, treatments, and cures for any diseases or conditions, as well as before changing your health care regimen. Do not reproduce, copy, reformat, publish, distribute, upload, post, transmit, transfer in any manner or sell any of the materials on this page without the prior written permission from myacare.com.
Dr. Anand Lakhkar is a physician scientist from India. He completed his basic medical education from India and his postgraduate training in pharmacology from the United States. He has a MS degree in pharmacology from New York Medical College, a MS degree in Cancer/Neuro Pharmacology from Georgetown University and a PhD in Pharmacology from New York Medical College where he was the recipient of the Graduate Faculty Council Award for academic and research excellence. His research area of expertise is in pulmonary hypertension, traumatic brain injury and cardiovascular pharmacology. He has multiple publications in international peer-reviewed journals and has presented his research at at prestigious conferences.
