Knock Knees (Genu Valgum): Symptoms, Causes, Diagnoses, and Treatment
Knock knees, or genu valgum, is abnormal knee alignment that is frequently seen in children, and less commonly in adults. Patients with genu valgum have an excessive inward alignment of their knees.
It’s usually a physiologic condition and part of your child’s normal growth process. Nevertheless, in adults and some children, it can be a sign of underlying illness and needs an orthopedist’s assessment.
What are knock knees?
Knock knees, also known as genu valgum, is a term used to describe incorrect knee alignment. When patients with knock knees stand up straight, the knees appear bumping together while the ankles and feet are far apart. Genu valgum can either be physiologic or pathologic:
- Physiologic knock knees are those normally seen during a child’s development. According to one study, up to 75% of children aged 3 to 5 have genu valgum. In most cases, knock knees go away on their own as your toddler grows, and their legs become straight by their 8th year.
- Pathologic knock knees are those that are severe, persist beyond 8 years of age, or start developing first during adulthood. These are almost always associated with other medical conditions like obesity, vitamin D deficiency, calcium deficiency, arthritis, or knee joint infection or trauma.
Treating pathologic knock knees early can help prevent future complications (like osteoarthritis) and deformities. Treatment options include corrective surgery, physical therapy, and lifestyle changes.
What are the symptoms of knock knees?
Knock knees have a typical appearance:
- Inward tilting of the knees
- Feet and ankles are up to 8 cm apart
- Feet that are rotated outward
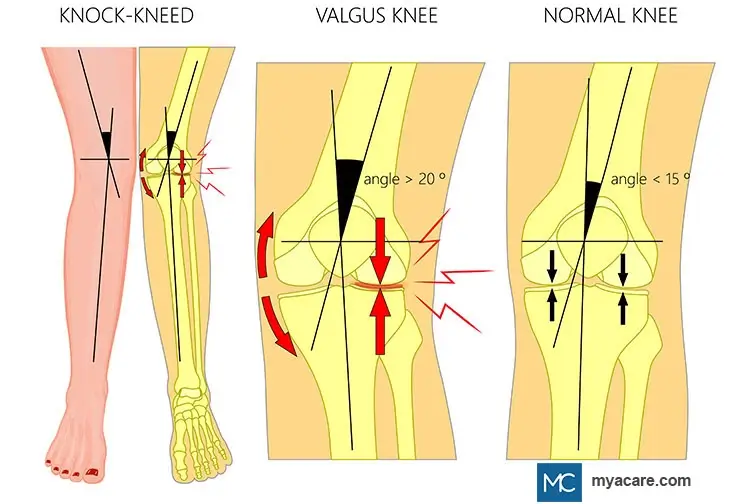
Patients with pathologic knock knees can have one or more of the following symptoms:
- Joint stiffness
- Knee pain
- Abnormal gait (walking pattern)
- Hip, feet, and/or ankle pain
- Unstable knees
- Walking or running difficulties
Since knock knees can ruin the body’s normal balance, other muscles and ligaments in the body will work extra hard to restore a normal posture. This can lead to their straining, and patients might develop pain in the ankles, feet, and hips. Other specific symptoms are usually related to the underlying cause of knock knees, like redness and swelling in case of an infection.
Should you worry about knock knees in your child?
Knock knees are a normal part of your child’s development process. The knee angles will normally change as your child grows. Infants usually have bowed legs until they reach 12-18 months of age. As they start walking by this age, their legs straighten. As they become 2-3 years old, the legs start tilting inward, which is the stage of “knock knees”. By about 7 or 8 years of age, the legs will have become straight again if your child’s growth is normal and undisturbed.
If your child follows a pattern similar to the one described, then it’s completely normal. However, if one or more of the following concerning features develop, you should get an orthopedist’s assessment to rule out any underlying conditions causing knock knees:
- If the knock knees persist after 7 years of age
- If the knock knees start before 2 years of age
- If one knee is obviously more affected than the other
- If your child has an abnormal walking pattern
- If your child has knee pain or hip pain
- Redness and swelling of the knees
- If your child is not growing normally in height
- If the knock knees are too severe
Adults who just recently started developing knock knees should not delay seeing an orthopedist, as it’s usually caused by a treatable medical condition.
How are pathologic knock knees diagnosed?
If you suspect that you or your child might have pathologic knock knees, medical evaluation is necessary. Your orthopedist will start by asking you for details about your medical history, surgical history, medications, and features of the disorder.
During the physical exam, the orthopedist will examine all the joints for any swelling or sign of disease, and try to pinpoint any pain. They will assess symmetry, leg length, and the degree of alignment. Depending on your physician’s suspicions, further testing might be ordered:
- X-ray imaging of the legs while standing sometimes helps confirm the diagnosis.
- MRI scanning might be ordered in cases where there’s a more elusive joint pathology.
- Vitamin D and calcium levels if deficiency is suspected
- Rheumatoid factor if arthritis is suspected
- Hormonal workup (thyroid and growth hormones) if growth delay in children is suspected
What are the causes of pathologic knock knees?
As opposed to physiologic knock knees seen during childhood, pathologic knock knees usually have one or more underlying causes:
- Rickets (soft bones due to vitamin D and calcium deficiency)
- Obesity
- Bone tumors
- Arthritis
- Osteomyelitis (bone infection)
- Kidney problems
- Metabolic illnesses
- Genetic and developmental abnormalities
- Injury to the bone’s growth plate during childhood
- Abnormal joint healing after trauma
Obesity can cause or exacerbate knock knees by putting more pressure on your child’s knees, leading to more inward tilting.
How do you treat knock knees?
Treating pathologic knock knees early on can prevent permanent deformity and later development of osteoarthritis (joint damage). Knock knees are treated by treating the causative medical condition along with some lifestyle changes and conservative therapies. In some cases, however, surgery might be the only option available to correct the deformity:
Treating the underlying condition
Treatment of knock knees starts with treating the underlying cause. For example, vitamin D and calcium supplements are given to those who have rickets. Anti-inflammatory and immune-modulating drugs are prescribed for rheumatoid arthritis.
Supportive treatment
Other lifestyle changes and non-surgical therapies might also help correct genu valgum:
- Weight loss: Excess weight might put more stress on your knee joints. If you are overweight or obese, your physician might suggest that you consider dieting and exercising to reach your ideal weight.
- Exercise and physical therapy: A certified physical therapist can teach you specific exercises to help stabilize your knees and straighten their alignment. Targeted exercises can also help improve your posture and strengthen your core muscles for better support.
- Orthotics: Insoles might help those with abnormal walk or foot pain. In children, leg splints might be helpful in guiding growth while minimizing knee angulation.
Surgical correction
Surgery is not usually needed to treat knock knees. However, in those with worsening knock knees, severe angulation, and those who are suffering from debilitating symptoms, surgery might be the only solution. Two surgical approaches are usually offered to correct genu valgum:
- Osteotomy: This is when an orthopedist cuts out a piece of bone to realign your knee joint at a normal angle. After removal of the bone piece, plates and screws are usually installed to keep the new alignment stable.
- Guided growth: This is usually offered to children who are rapidly growing. Plates and screws are surgically fixed on the sides of the knee joint. The screws will be manipulated by the surgeon in subsequent procedures to adjust knee alignment as the child grows. This treatment protocol is usually done over a period of 12 months, during which multiple adjustments are done.
In most children, knock knees should not have you worried. However, in adults, older children, and young children with concerning features, knock knees can be a sign of an underlying disease. Treating the underlying condition, exercising, and getting physical therapy can reduce knock knees and prevent further deformity. In those who have severe knock knees and fail to respond to non-surgical treatment, surgery is an effective option.
To search for the best Orthopedics Healthcare Providers in Croatia, Germany, India, Malaysia, Singapore, Spain, Thailand, Turkey, Ukraine, the UAE, UK and the USA, please use the Mya Care search engine.
Dr. Mersad is a medical doctor, author, and editor based in Germany. He has managed to publish several research papers early in his career. He is passionate about spreading medical knowledge. Thus, he spends a big portion of his time writing educational articles for everyone to learn.
Sources:
Featured Blogs



