Artificial Urinary Sphincter: A Cure for Incontinence in Men

After prostate surgery, many men develop urinary incontinence. It can become embarrassing and interfere with the quality of life if not properly dealt with.
In most cases, urinary incontinence after prostate surgery resolves on its own. In some men, however, it persists and becomes a real burden.
The artificial urinary sphincter is a prosthetic device that’s implanted around the urethra to prevent urine from leaking out involuntarily. This device allows the patient to control urination with the click of a button.
It is considered the gold standard treatment for urinary incontinence after prostate surgery if all other measures fail.
Keep reading to learn more about artificial urinary sphincters and how they work!
What is Stress Urinary Incontinence?
Urinary incontinence is the involuntary loss of urine. Stress incontinence is a major type of urinary incontinence that can occur in both men and women.
Stress incontinence is when urine leaks as a result of increased abdominal pressure - when you laugh, sneeze, or cough for example.
In women, stress urinary incontinence usually happens as a result of aging or as the long-term aftermath of childbirth. Both of these things damage the natural urinary sphincter and surrounding nerves.
In men, Stress incontinence usually happens after prostate surgery (prostatectomy or TURP) due to nerve damage or direct damage to the natural urinary sphincter.
Mechanism of Stress Incontinence
In order to understand how the artificial urinary sphincter works, you first need to learn a little more about the anatomy and physiology that goes into urination.
Urine goes down from the kidneys to the bladder to be stored. When you want to urinate, the urine goes down from the bladder into the urethra, which is a muscular tube that leads urine outside of your body.
Right below the bladder, and just around the first part of your urethra is the “urinary sphincter”. This is a strong circular muscle responsible for holding the urine inside the bladder and preventing it from going out.
The problem is that the natural urinary sphincter is located inside the prostate. This is why prostate surgery commonly insures this sphincter and makes it incompetent.
When the sphincter is incompetent for any reason (whether it is prostate surgery or not), then it will fail to stay closed against increased pressure. When you sneeze, jump, or laugh, you will be putting pressure on your bladder. If your urinary sphincter is incompetent, then urine will leak out. This is stress urinary incontinence.
How Does an Artificial Urinary Sphincter Work
The goal of an artificial urinary sphincter is to replace the function of your incompetent natural urinary sphincter. It prevents urine from leaking out unless you want to urinate.
An artificial urinary sphincter (AUS) is made of 3 parts connected together with plastic flexible tubes:
- A cuff: this goes around your urethra and shuts it tight
- A reservoir balloon: this balloon contains sterile saline (saltwater) and is implanted in your pelvis
- A pump: the pump is implanted in your scrotum and has an activation button that you can palpate and press when you want to urinate
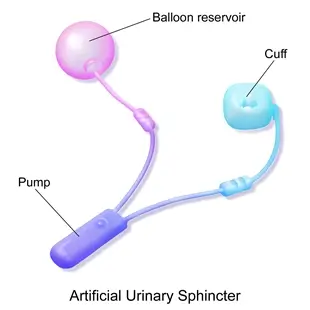
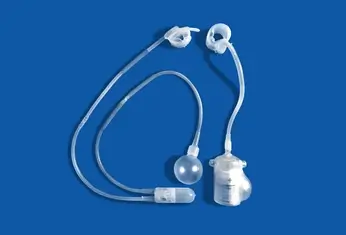
When you want to urinate, you will palpate the pump in your scrotum and press the activation button. The pump will move the fluid within the system to loosen the cuff around your urethra (the fluid goes to the reservoir balloon). Once the cuff is loosened, urine will freely flow out and you can empty your bladder
Once done, the cuff will automatically regain its pressure within a couple of minutes and re-shut the urethra tight. You are continent again.
Who is a Candidate for an Artificial Urinary Sphincter?
The artificial urinary sphincter is not for everyone. It is currently only indicated for the treatment of stress urinary incontinence that develops in men after prostatectomy and TURP.
The AUS can be used to treat other forms of incontinence as well, however, it is not considered a standard treatment yet.
Men who develop urinary incontinence after prostate removal usually regain their continence within a year of their surgery. This is why an artificial urinary sphincter is only offered after a full year passes.
How Effective is an Artificial Urinary Sphincter?
The goal of a urinary sphincter implant is to cure incontinence or at least significantly reduce it to improve the quality of life.
According to one review done in 2016, the success rate of artificial urinary sphincters ranged between 61% and 100%. Moreover, patient satisfaction with their urinary sphincter implants ranged between 80% and 90%.
Even after several years of follow up, the artificial urinary sphincter maintains a very acceptable success rate. According to one study done in 2009, the success rates of AUS were at 72% after 5 to 7 years of follow-up.
Complications of Artificial Urinary Sphincter
Artificial urinary sphincters are not without risks or complications. After all, it is an implantable foreign body.
According to one study, the overall complication rate is 37%, and many of these cases require surgical revision.
The most common complications reported with artificial urinary sphincter include:
- Device infection: this can require device removal and long term antibiotic therapy
- Mechanical failure: the AUS is indeed durable, but its effectiveness will eventually start to decrease after a few years eventually requiring adjustment or replacement.
- Urethral erosion and atrophy: the constant pressure of the cuff on your urethra can lead to erosion and thinning of the urethra. This can require cuff repositioning or pressure adjustment to maintain continence.
In general, it is estimated that up to 26% of men need surgical revision within 10 years of having an artificial urinary sphincter implanted.
Outlook
Urinary incontinence in men can be very stressful, and an important cause of embarrassment and social distress.
If you have stress incontinence after prostate surgery, your continence might improve within a year. If not, there are several conservative and surgical treatments that can help reduce incontinence.
An artificial urinary sphincter is an excellent choice in men who are incontinent after prostatectomy. It is a permanent solution for this problem. It’s always best to discuss in more detail with your urologist and see if you qualify, as well as the risks and benefits.
To search for the best healthcare providers that offer Prostate Surgery, Croatia, India, Malaysia, Spain, Thailand, Turkey, United Arab Emirates, United Kingdom, and the United States, please use the Mya Care search engine.
Dr. Mersad is a medical doctor, author, and editor based in Germany. He has managed to publish several research papers early in his career. He is passionate about spreading medical knowledge. Thus, he spends a big portion of his time writing educational articles for everyone to learn.
Sources:
Featured Blogs

Medically Induced Coma: What It Is, How It Works, Who Benefits, and Recovery Outcomes


