Fish Skin for Burn Wounds: The Future Wound Dressing?
Originally Authored by Dr. Mersad Alimoradi - July 29, 2021
Medically Reviewed and Updated by Dr. Rae Osborn, Ph.D. - July 16, 2025
According to the WHO, nearly 180,000 individuals die of burn injuries each year. More than 11 million people suffer severe burns and require medical care. Those are big numbers.
Burns are a very common type of injury that can lead to scarring, deformity, disability, and death. Doctors and researchers are always working on developing better ways to treat burn victims and give them the best functional and cosmetic outcomes.
Impeccable wound care and skin grafting have been the cornerstone of burn wound treatment. In recent years, researchers in Brazil have started using fish skin as a biological dressing to help heal wounds faster and reduce pain.
The Tilapia fish skin is currently being studied and used in Brazil, and it has shown excellent results. It is cheap, reduces pain, and speeds up healing. So, will fish skin be the new trend in treating burn wounds?
How It Started
The main reason behind using fish skin was the lack of enough donor human skin grafts in a developing country like Brazil. Compared to more advanced countries, like the USA, Brazil has a less robust organ donation program. Hence, many burn victims do not receive skin grafts or have to pay astronomical amounts of money to get a donor graft.
The Tilapia fish skin is very cheap to produce. Tilapia are very commonly grown in fish farms all around Brazil, and the skin is a waste product that is usually thrown away. This means that it is very cheap to acquire and develop for medical use.
And this is exactly what researchers at the Federal University of Ceará did.
They used Tilapia fish skin to treat burn wounds in a 23-year-old Brazilian man who was injured by a gunpowder explosion. The fish skin was applied to his arms and hands and then covered with gauze. The treatment led to fast and very effective healing.
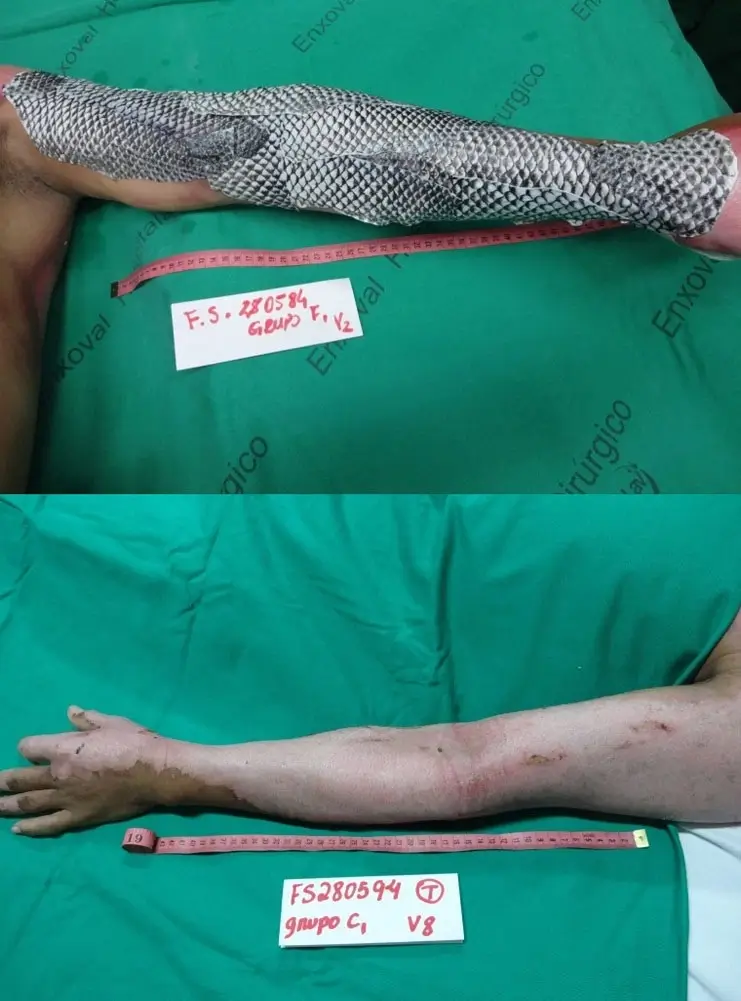
Tilapia fish skin applied onto the left arm (Image 1). The results after 17 days (Image 2).
Lima-Junior EM, de Moraes Filho MO, Costa BA, et al. Innovative treatment using tilapia skin as a xenograft for partial thickness burns after a gunpowder explosion. J Surg Case Rep. 2019;2019(6):rjz181. Published 2019 Jun 14. doi: 10.1093/jscr/rjz181
Why Fish Skin?
This is probably the first question that comes to mind when hearing about the successful treatment outcome.
The skin of the Tilapia fish is very similar to that of humans, and maybe even better. It was observed to improve the healing process and reduce pain effectively in burn victims. But why is that?
Here are the things that make fish skin great for burn wound healing:
- Contains high levels of collagen type 1, which has high tensile strength and resistance, and promotes healing by encouraging the development of structural cells in the wound.
- Contains a large amount of Omega-3 fatty acids, which have great antibacterial and antiviral properties, making fish skin strongly protective against infection.
- Contains a wide variety of amino acids, which stimulate cell and tissue regeneration, reduce inflammation, fight off bacteria, and protect the nerve endings.
- Contains special healing peptides (tilapia piscidin-3 or TP3) that speed up cell proliferation, remodeling, and maturation of infected wounds.
- Adheres firmly to the wound
- Holds moisture very effectively
- Cheap and readily available
All these characteristics of fish skin make it a promising tool for treating moderate and severe burns. It can replace regular gauze dressing and improve the outcomes. Doctors in Brazil have been able to demonstrate this through their research (see below).
How it Works
Tilapia fish skin needs to be processed to make it suitable to apply on the wounds of burn victims.
First, the skin is collected, cleaned, treated chemically (sometimes with silver nanoparticles), and irradiated. After that, it is tested to ensure it is sterile, and finally, it is placed in specialized packaging ready to be used.
- The fish skin is used as a biological dressing for the wound. It is applied directly on the burn wounds to cover all the exposed tissue and part of the healthy skin.
- There is no need to add any extra creams (like silver or sulfadiazine)
- The fish skin is covered by sterile gauze
During the healing process, the Tilapia fish skin will adhere firmly to the exposed skin. This provides excellent protection against external insults. The numerous proteins and fatty acids will infiltrate the wound and stimulate healing.
For superficial wounds, there might be no need to change the fish skin. It can be left there until the skin regenerates on its own and the fish skin sloughs off.
For deeper wounds that require weeks to heal, fish skin dressings might need to be repeated a few times before the skin fully heals. Nevertheless, dressing changes are much less often than with regular gauze and creams.
Fish Skin Compared to Other Xenografts
There are advantages of using fish skin for grafts compared to tissue derived from cadavers, pigs (porcine), or cows (bovine). Cow and pig skin could transmit diseases, such as bovine spongiform encephalopathy (BSE) or foot-and-mouth disease.
In the past, cadaver skin has been used to treat burn wounds. An advantage of fish skin over cadaver skin is the large amounts of omega-3s found in fish that are only present in trace amounts in cadaver skin. There is also less chance of viral transmission if fish skin is used rather than cadaver skin.
Fish skin also has greater absorption efficiency and bioavailability.
Latest Research
New research has recently demonstrated the great benefits of fish skin in treating burn wounds. Fish skin has been shown to be superior to routine management with gauze and burn creams.
The research group that originally suggested Tilapia fish skin as a possible treatment for burn wounds published the results of a clinical trial that involved 115 burn victims in Brazil.
The Phase III results, published in the journal “Plastic and Reconstructive Surgery” in May 2021, showed that using fish skin for burns:
- Speeds up the healing process (re-epithelialization)
- Reduces the frequency of wound dressing changes
- Reduces pain and the need for painkillers
- Reduces the costs of treatment significantly
Advancements in the use of fish skin
Further research has been done on using and modifying fish skin for wound treatment.
- Acellular Fish Skin Grafts
Acellular fish skin (AFS) is tissue where the cells have been removed. It is porous and supports the attachment and growth of cells in 3D. AFS still contains collagen and omega-3 fatty acids, which promote stem cell differentiation and wound healing. AFS is used as a matrix to which cells attach, promoting the healing of burn wounds.
- Products Derived from Extracted Fish Skin Components
Extracts from fish skin can be used to heal wounds. Collagen extracted from Tilapia increases skin cell growth and differentiation. Natural collagen has high tensile strength and high biocompatibility, and so can be made into sponges and patches, and used for skin grafts and other tissue engineering applications. For instance, collagen patches can be used to deliver certain medications, such as anti-inflammatories.
Tilapia skin can be used to make a hydrogel after being combined with methacrylic anhydride (MA). Growth factors were added, and the hydrogel was shown to help full-thickness wounds heal.
- Isolated Macromolecules and Bioactive Compounds
Tilapia fish skin also has alanine and proline, which help form collagen. The high thermal stability of collagen from fish could be used as a substitute for human collagen. The collagen peptides from the skin can be used in various applications since they reduce oxidative stress and have antibacterial properties. Omega-3 fatty acids from fish skin, particularly eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), help reduce inflammation.
- Enhanced and Hybrid Fish Skin Dressings
Fish skin can be infused with antimicrobial agents, such as silver nanoparticles. Sterilizing the skin with silver means less of the collagen is destroyed. Adding silver nanoparticles also protects fish skin for use in wound dressings.
Advanced hybrid skin patches made of acellular skin grafts and chitosan have been developed. Vascular endothelial growth factor was added to the chitosan, making it antibacterial and promoting the growth of blood vessels. Using a rat model, this patch helped tissue regenerate in full-thickness wounds.
Conclusion
Fish skin is emerging as a potential and affordable option for burn wound care, particularly in settings with limited access to donor grafts. With its rich composition of collagen, omega-3 fatty acids, and healing peptides, it not only accelerates wound healing but also reduces pain, the frequency of dressing changes, and overall treatment costs. As clinical evidence continues to grow, fish skin, especially in its enhanced and hybrid forms, may become a vital component in the global standard of care for burn injuries.
To search for the best Dermatology Healthcare Providers in Croatia, Germany, Greece, India, Malaysia, Singapore, Slovakia, Spain, Thailand, Turkey, Ukraine, the UAE, UK, the USA, please use the Mya Care search engine.
The Mya Care Editorial Team comprises medical doctors and qualified professionals with a background in healthcare, dedicated to delivering trustworthy, evidence-based health content.
Our team draws on authoritative sources, including systematic reviews published in top-tier medical journals, the latest academic and professional books by renowned experts, and official guidelines from authoritative global health organizations. This rigorous process ensures every article reflects current medical standards and is regularly updated to include the latest healthcare insights.

Dr. Rae Osborn has a Ph.D. in Biology from the University of Texas at Arlington. She was a tenured Associate Professor of Biology at Northwestern State University, where she taught many courses to Pre-nursing and Pre-medical students. She has written extensively on medical conditions and healthy lifestyle topics, including nutrition. She is from South Africa but lived and taught in the United States for 18 years.
Sources:
Featured Blogs

Medically Induced Coma: What It Is, How It Works, Who Benefits, and Recovery Outcomes


