From Orthognathic to Orthofacial Surgery: New Perspectives for Facial Aesthetics

The misalignment of the upper jaw (maxilla) with the lower jaw (mandible) can lead to an abnormal bite and an uneven facial appearance.
Orthognathic jaw surgery helps correct the shape and alignment of the jaw and its functions. However, many patients seeking jaw realignment surgery are primarily concerned about the aesthetic end result.
This concern prompted the development of orthofacial surgery, which focuses on facial aesthetics such as symmetry, and projection of the face, and jaw function. Orthofacial surgery combines other facial cosmetic surgery procedures, including genioplasty and rhinoplasty, with orthognathic surgery to maximize the aesthetic results.
Orthognathic vs. Orthofacial Surgery
Orthognathic surgery is a set of jaw reshaping procedures to repair defects in the upper (maxilla) and lower (mandible) jaws.
The abnormal positioning or size of the upper and lower jaws can cause orthodontic malocclusion (an abnormal bite). Realignment with jaw corrective surgery aims to correct malocclusion that cannot be improved by straightening the teeth alone (orthodontics).
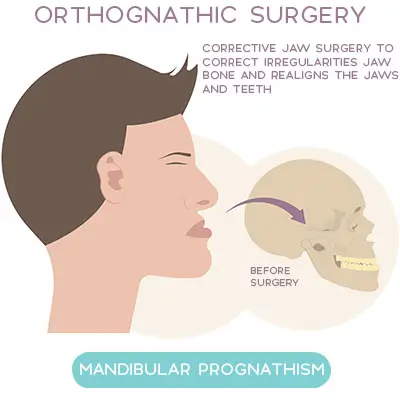
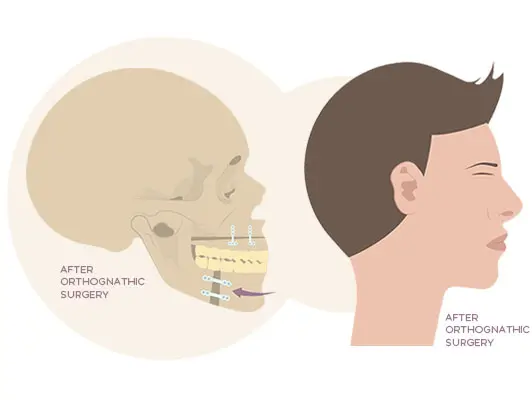
Orthofacial surgery is based on orthognathic surgery with a special focus on how reshaping the jaw affects the cosmetic appearance of the face. Orthofacial surgery addresses both the functional and aesthetic concerns of patients with jaw problems. It involves the manipulation of the jaw bones and the underlying soft tissue to enhance the cosmetic features of the face, including facial symmetry and projection.
Surgical Techniques in Orthofacial Surgery
Advanced orthofacial surgery techniques include:
- The repositioning of the mandible (lower jaw) and maxilla (upper jaw)
- In some cases, secondary procedures of the chin and nose, fat transfer, and/or lifting procedures to maximize the final facial aesthetic result. These procedures also aim to harmonize facial features by taking into account the changes caused by the readjustment of the jaw.
Bimaxillary surgery
Bimaxillary surgery, also known as maxillomandibular surgery or double jaw surgery, is a surgical procedure that repositions both the upper jaw (maxilla) and lower jaw (mandible).
Bimaxillary orthognathic surgery is a combination of upper and lower jaw surgical procedures:
- Le Fort I osteotomy (maxillary osteotomy): The maxillary bone above the upper teeth is cut so that the entire upper jaw can be moved forward, backward, or rotated either clockwise or anticlockwise. The maxillary bone can also be shortened (by shaving or removing excess bone) or lengthened (by bone grafting).
- Bilateral sagittal split osteotomy (mandibular osteotomy): The mandibular bone is cut behind the molars. The lower jaw can then be moved backward or forward, rotated, shortened, lengthened, or centered and leveled to straighten it into a more balanced and functional position.
Double jaw surgery is used to correct:
- Class II bite (overbite): The upper front teeth extend farther than the lower front teeth. As a result, the face looks short because the lower jaw appears retracted. An overbite can be caused by an over-protruding upper jaw or a receding lower jaw.
- Class III bite (underbite): The lower teeth extend in front of your upper teeth. This can make the lower jaw look too big or too long. An underbite is usually caused by an over-protruding lower jaw or under-protruding upper teeth.
- Open bite: The top and lower teeth don’t come together at the front or in the posterior segment when you bite down, making them look open. An open bite can be caused by the misalignment of the upper jaw with the lower jaw.
- Crossbite: The top and lower teeth don’t close on each other in the correct position making the bite off-center.
- Facial asymmetry: Commonly attributable to genetic causes, and can also include, asymmetry of the chin, the eye area, or an underdeveloped side of the face due to muscular atrophy.
Realigning the upper and lower jaw at the same time can harmonize the mid and lower thirds of the face and achieve proper occlusion. It can also improve symptoms of moderate or severe obstructive sleep apnea caused by jaw misalignment.
Surgeons use bimaxillary surgery advancements to rotate the entire jaw in a clockwise or counterclockwise position and attain maximum functional and aesthetic results.
Intraoral cervical lift
After repositioning the mandible and the maxilla, the facial features can be further enhanced with an intraoral cervical lift. This minor surgical technique is done to manipulate the soft tissue under the jaw.
By using the same incision made during mandibular osteotomy, the surgeon pulls the soft tissue in the muscle at the back of the jaw (platysma muscle). The soft tissue is then tightened around the mandible.
The soft tissue and muscles under the chin are lifted and tightened, giving the neck a better definition and improving the projection of the face.
Genioplasty (chin surgery)
Chin reshaping surgery can be done in combination with jaw reshaping surgery to improve the overall appearance of the face.
If the chin is too prominent, the surgeon will cut above it, remove a small piece of bone, and move the whole chin inward.
Genioplasty can also be used to correct a small chin which often accompanies a receded lower jaw. The chin can be restructured by bringing it forward to become more protruding and pointed. As with the jaws, a genioplasty allows to lower, shorten, rotate, level, and center the chin bone.
Rhinoplasty
It can be combined with jaw realignment during orthofacial surgery to reshape the nose so it better fits the newly shaped jaw. It is important during planning to take into consideration the changes in the nose that the repositioning of the maxilla will bring about.
Benefits of Orthofacial Surgery
Although orthofacial surgery aims to improve patients' appearance by realigning their jaws, it is also a functional procedure that corrects jaw functions and related airway issues. The advances in orthofacial surgery have made it possible to:
- Fix facial aesthetic problems (facial symmetry, projection, and profile)
- Correct orthodontic malocclusions (underbite, overbite, cross bite, open bite)
- Fix airway problems (such as obstructive sleep apnea)
- Improve speech that has been hindered by jaw misalignment

Dr. Federico Hernández Alfaro is a Professor of Oral and Maxillofacial Surgery at the Universitat Internacional de Catalunya (UIC) and Director of the Institute of Maxillofacial Surgery and Implantology at Quirónsalud Teknon Medical Center in Barcelona, Spain. Dr. Federico Hernández Alfaro is a world leader in the field of orthognathic surgery, completing approximately 200 such cases each year. Pioneering new methods, Dr. Alfaro and his research team have developed and published several innovative techniques that allow for minimally invasive approaches which translates in more accuracy, shorter surgical times, and a better and shorter recovery for the patient.

Quirónsalud Teknon Medical Center is one of the leading private sector hospitals in Spain, delivering high-quality medical care with personal attention and utilizing the latest technologies.
The Maxillofacial Institute in Barcelona, Spain, has an excellent team of oral and maxillofacial surgeons, led by Dr. Federico Hernandez Alfaro, with extensive training in both craniofacial surgeries as well as traditional cosmetic procedures. Our team of doctors uses state-of-the-art imaging techniques and the most advanced surgical procedures to treat malocclusion and give the best facial cosmetic results possible.
The Maxillofacial Institute is one of the first centers in the world to implement the concept of orthofacial surgery. For years, the Institute has used a more holistic approach to fix jaw alignment problems while providing unparalleled facial aesthetic results.
The Institute has a team of experts with specialized training and experience in different orthofacial procedures. They use minimally-invasive techniques to realign the jaw with less surgical time and minimal incisions.
The use of advanced imaging techniques for orthofacial planning, such as a state-of-the-art intraoral scanner, low radiation cone-beam computed tomography (CBCT), and the latest 3D software, allows our surgeons to carefully and precisely plan the orthofacial surgeries while minimizing any errors or complications.
Sources:
Featured Blogs



