Melanoma: Definition, Diagnosis, and Treatment
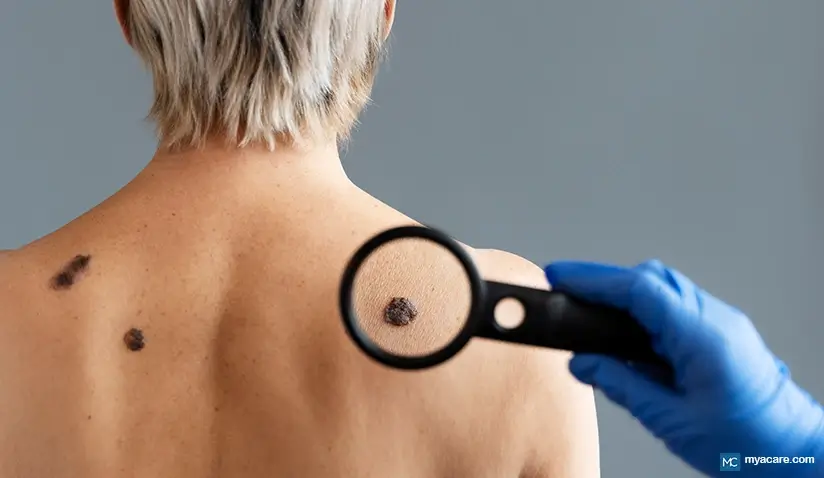
Melanoma is the most dangerous type of skin cancer. It arises from melanocytes, which are cells responsible for giving color to your skin (melanin-producing cells).
Although it’s skin cancer, melanoma can still sometimes form in the eyes and other regions of the body (e.g. throat).
Melanoma is believed to be caused by excessive UV light exposure, although genetic factors are believed to play a role in its development.
Starting off as a suspicious mole, it can grow rapidly and penetrate deeper into your body, even spreading to internal organs. Knowing the possible signs of skin cancer can ensure the symptoms are detected and treated before it can spread.
If you notice a mole that wasn’t there before, it is recommended that you see a dermatologist, since early diagnosis of melanoma increases the chances of effectively curing the tumor
What Is Melanoma?
Melanoma is a malignant skin cancer that is strongly associated with sun exposure; mainly UV exposure. It develops from melanocytes, which are special cells that produce melanin, a hormone responsible for the pigmentation of the skin, eyes, and hair.
Also known as malignant melanoma or cutaneous melanoma, this cancer can spread to other parts of the body, in which case it’s referred to as metastatic melanoma.
The American Cancer Society believes that almost 106,110 new cases of melanoma will be diagnosed in the US in 2021 alone, with 7180 expected deaths.
Melanoma is not the most common skin cancer but is the one associated with the highest mortality rates, especially if detected late at an advanced stage.
Symptoms Of Melanoma
Melanoma can produce a wide range of symptoms with the first symptoms often being a suspicious mole.
If you develop a new mole that matches the following characteristics or have an old mole that now meets the following criteria, it is recommended to see a dermatologist:
A: Asymmetric or irregular in shape.
B: Border of the mole is not sharply demarcated..
C: Color of the mole is changing/has changed.
D: Diameter of the mole has changed or keeps changing.
E: Evolving appearance of the mole.
Remember the ABCDEs of melanoma to know when to see a doctor. If you have a mole showing such characteristics, then you should not delay visiting a dermatologist or your GP.
Causes Of Melanoma
Healthy new cells develop by pushing older cells to the skin’s surface, where they die and fall off.
With skin cancers, like melanoma, things are different. The cancerous cells don’t die and fall off. They continue multiplying and form a tumor. Cancerous cells are cells that have developed damaged DNA or harmful mutations due to a number of reasons. This damage leads to uncontrolled cell multiplication and the development of melanoma.
The exact cause of the damaged cells and melanoma is not clear. Doctors believe that exposure to ultraviolet (UV) radiation is responsible for melanoma cells development. Nevertheless, it is likely that a combination of various other factors come together to make us susceptible.
Moreover, melanomas can also develop in parts of your body that sunlight does not reach. This points towards other potential causes that have not yet been discovered.
Risk Factors Of Melanoma
While there is no one cause of melanoma, skin cancer can be caused by certain environmental and genetic factors. Understanding whether you are at a high risk of melanoma is the first step for preventing adverse outcomes.
These risk factors increase your probability of developing melanoma:
- Excessive UV ray exposure: Constant exposure to UV radiation, whether it’s from the sun or from tanning beds, can increase your risk of developing melanoma.
- Presence of many or irregular moles: Having many moles on your body puts you at a greater risk for melanoma, especially if these moles look irregular.
- Fair skin: Caucasians and light-skinned individuals are at higher risk for melanoma than darker-skinned individuals. The less melanin you have, the more you’re at risk of developing melanoma. Darker-skinned people can still develop melanoma, although cases are relatively low.
- History of sunburns: Increased number of sunburns means an increased risk of melanoma. Sunburns can dampen your skin’s protective mechanisms and increase the likelihood of mutations.
- Family history or personal history of melanoma: If you or someone in your family has already had melanoma, you are more likely to develop melanoma or get it again.
How Is Melanoma Diagnosed?
Diagnosis involves a series of steps:
- Clinical Evaluation and History Taking: Diagnosis of melanoma skin cancer initially begins with your doctor asking whether you have possible risk factors for melanoma, such as tanning and sunburns, and if you or any of your family have a history of melanoma or other skin cancers. During the physical exam, your dermatologist performs the ABCDE evaluation of the suspicious mole.
- Skin Biopsy: Your doctor may recommend a biopsy of the mole to determine whether it is melanoma. There are different types of biopsies your doctor can suggest depending on the extent of your condition. Most of the time, your doctor will opt for the procedure that removes the entire growth (excisional biopsy).
- Histopathological Examination: Biopsies are sent to a pathologist to be studied under the microscope. If your diagnosis is melanoma, the next step will be to determine the extent of the skin cancer and see if it has reached the deeper layers of the skin. The staging and classification of melanoma cells are done by a pathologist so that an appropriate therapy plan can be formed and initiated.
- Lymph Node Biopsy: Your dermatologist may also check if your melanoma has metastasized or spread to nearby lymph nodes by doing a sentinel lymph node biopsy. If the biopsy shows cancer cells, then a lymph node dissection may be performed. This procedure is the removal of all lymph nodes near the melanoma.
Stages Of Melanoma
Stage 0: Melanoma is localized in the epidermis and has not spread to nearby lymph nodes or deeper body parts. Stage 0 is a non-invasive stage called melanoma in situ.
Stage 1: The cancer is no more than two millimeters thick and may or may not be ulcerated. Stage 1 melanoma has penetrated the outermost layer into the next layer of skin.
Stage 2: The tumors go deeper than one millimeter and might or might not be ulcerated. Melanomas thicker than four millimeters are more at risk of spreading. Ulceration can also bring melanoma to the next stage.
Stage 3: These tumors include those that have spread from the primary tumor but not yet to the lymph nodes and those that have spread to the local lymph nodes. Satellite tumors or melanomas that have spread to nearby skin and tissue but not the lymph nodes are also included.
Stage 4: The melanoma has metastasized to distant lymph nodes and organs, such as the brain, lungs, liver, and gastrointestinal tract. Stage 4 tumors can be of any thickness and may or may not be ulcerated.
Types of Treatment
Therapy of melanoma includes several combination therapies and adjuvant therapy options such as:
Surgical excision is the primary treatment option for treating small, early-stage melanomas. Your surgeon may treat larger melanomas with chemotherapy before and/or after surgery to increase the cure rate.
During surgery, your surgeon may also remove lymph nodes if they suspect that they contain cancer cells.
In some cases, small cutaneous melanomas may be completely removed through the excisional biopsy alone, and no further treatment is required. The pathologist that studies the sample can determine if the biopsy alone has completely removed the tumor.
- Chemotherapy: Chemotherapy entails the use of specific drugs to destroy cancer cells and inhibit their growth. Chemo can be used to treat advanced melanoma stages. This may be the only treatment, or your doctor may use it along with surgery to increase the chances of complete remission.
Chemotherapy is often employed after other treatments have been tried because newer forms of therapy are considered more effective.
- Targeted Therapy: Targeted drugs are different from chemotherapy drugs, which attack rapidly dividing cells. Targeted drug therapy targets specific parts of the melanoma cells that make them unique (compared to normal cells). By accurately targeting these unique receptors, targeted drugs can effectively kill cancer cells and shrink the tumor.
This therapy is preferred if the melanoma has spread to internal organs and lymph nodes in the body.
- Immunotherapy: Your immune system often can’t destroy cancer cells because these cells produce a protein that helps them blend in with normal, healthy cells. Immunotherapy is a drug therapy that encourages your immune system to recognize and destroy cancer cells.
This treatment is recommended for melanoma that has metastasized or melanoma that can’t be entirely removed through surgery.
Radiation therapy includes the use of high-energy X-ray radiation directed at melanoma cells to burn and destroy them. The most common type of radiation that treats melanoma is called external beam radiation. This method focuses an external source of radiation onto the melanoma to burn it.
Doctors use radiation therapy when surgery cannot be done. Sometimes, radiation treatment is recommended after surgically removing metastatic lymph nodes.
Outlook of Melanoma
Melanoma survival rates depend on the stage. Early diagnosis is usually related to increased rates of curability. But melanoma must be identified and treated without delay.
If you see a new and suspicious mole on your skin, have a dermatologist examine it as soon as possible. Remember the ABCDE method to help you determine whether your mole is a melanoma.
With the improvement of melanoma treatment over time, people diagnosed with melanoma now have a better outlook. Remember to stay proactive and keep an eye on the changes in your skin.
Frequently Asked Questions about Melanoma
- Is melanoma always fatal?
Melanoma is the most common type of skin cancer that can be completely curable if diagnosed early. However, after it spreads to the deeper layers of the skin and becomes metastatic melanoma, you may require combination therapy for treatment.
- How do you get melanoma?
Excessive UV exposure from sunlight and tanning beds increases the risk of melanoma significantly. Sun exposure and repetitive trauma can destroy normal skin cells and result in cancer development.
- How fast does melanoma spread?
Melanomas develop quickly and can become life-threatening in less than six weeks. They can spread to deeper layers of your skin, and then to internal organs, even the distant organs, quite quickly. Metastatic melanomas are also harder to treat.
- Where does melanoma spread first?
Melanomas usually spread to the nearby lymph nodes first as they drain cancer cells directly into themselves. These lymph nodes are called sentinel lymph nodes and are tested via sentinel lymph node biopsy. Lung, brain, liver, bone, and intestinal metastases are common with melanoma.
- Can I have melanoma and not know it?
Melanomas, based on their type, have different rates of growth. Cutaneous melanomas grow fast, spreading within weeks, whereas radial melanomas take decades to develop and grow. It is recommended that you get any suspicious moles checked for melanoma as soon as you get the chance.
To search for the best Oncology healthcare providers in Germany, India, Malaysia, Singapore, Spain, Thailand, Turkey, Ukraine, the UAE, the UK and the USA, please use the Mya Care search engine.
To search for the best healthcare providers worldwide, please use the Mya Care search engine.
Dr. Mersad is a medical doctor, author, and editor based in Germany. He has managed to publish several research papers early in his career. He is passionate about spreading medical knowledge. Thus, he spends a big portion of his time writing educational articles for everyone to learn.
Sources:
Featured Blogs



