Dropped Metatarsal: Causes, Symptoms, and Treatment

Continuous pain in the ball of the foot, or Metatarsalgia, can affect your daily life. It can impact your ability to exercise, perform your job, or enjoy physical activities. One of the most common causes of foot pain, Metatarsalgia, is more prevalent in women and the elderly as per research.
There are various conditions that can cause metatarsal pain, including a stress fracture, Achilles tendon rupture, a broken foot, a broken toe, or foot overuse injuries. Another common cause of metatarsalgia is a dropped metatarsal bone.
When one of the metatarsal bones is misaligned, it becomes pressured and stressed more than the other bones. This leads to pain and inflammation in that area. People with a fallen metatarsal experience sharp and aching pain in the ball of the foot that worsens after physical activity.
An orthopedist or podiatrist can diagnose if a dropped metatarsal is the source of your metatarsalgia and then recommend the proper conservative or surgical treatment for your condition.
What is Dropped Metatarsal?
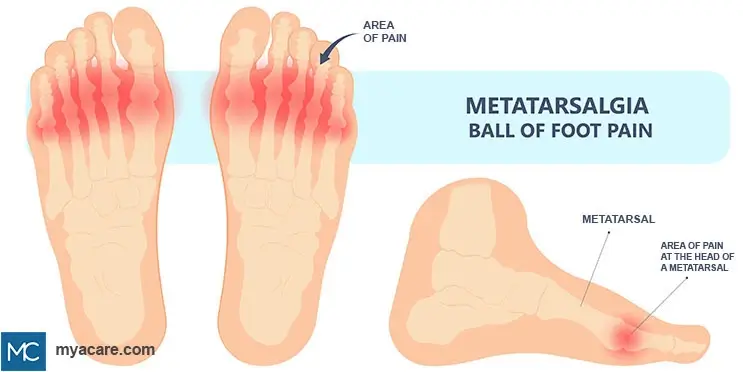
The metatarsal bones are five long bones extending from the ball of the foot connecting your toes with your ankle bones. Sometimes this area of the foot becomes painful and inflamed; a condition called Metatarsalgia.
Although a lot of things can cause metatarsalgia pain, the most common cause is a dropped metatarsal (also known as dropped metatarsal head). Metatarsal drop is the condition where one of the five metatarsal bones is lower than the others near the ball of the foot.
This uneven positioning of metatarsal bones causes an unbalanced distribution of weight and pressure across the foot bones. As a result, callus forms under the dropped metatarsal because of the pressure, ultimately leading to metatarsal foot pain.
What Are the Symptoms of Dropped Metatarsal?
People who experience metatarsalgia because of a fallen metatarsal head usually complain of:
- Burning pain in the ball of the foot
- Pain around the big toe or around the 2nd, 3rd, or 4th toes
- Foot pain that worsens with physical activity or walking barefoot
- Pain in the feet that gets better when your rest
- A sensation of walking on pebbles or marbles
Persistent foot pain can cause you to limp or prevent you from performing daily activities.
If you have ongoing metatarsal pain, you should make an appointment with your doctor to get a proper diagnosis and effective treatment.
What Causes a Dropped Metatarsal?
Dropped metatarsal is a common hereditary condition. Most likely, a metatarsal drop can be genetically passed down to you from your parents.
Doctors also believe that overpronation of the foot can also be a cause. Overpronation is when the foot arches become flattened, thus straining some of the supporting muscles and tendons.
Consequently, too much pressure on one of the metatarsal bones causes it to drop.
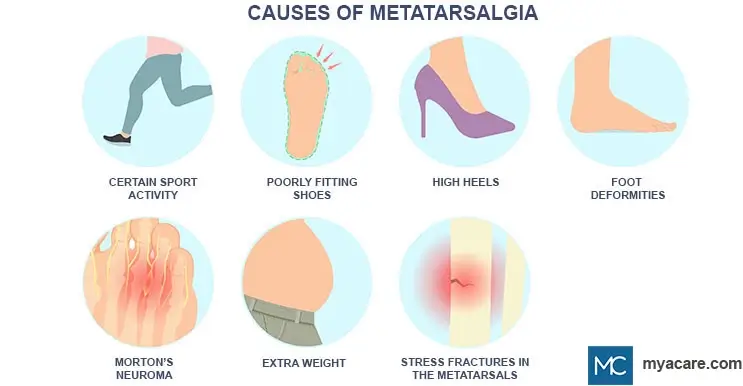
What Are the Risk Factors of Dropped Metatarsal?
You are more likely to have a fallen metatarsal in the following cases:
- If you have rheumatoid arthritis or osteoarthritis
- If you’ve suffered a sports-related foot injury (e.g. Achilles tendonitis, plantar fasciitis, stress fracture in the metatarsals)
- If you undergo intense physical training that overuses the feet
- If you work or exercise while standing on hard surfaces (e.g. cement, tile)
- If you often wear high heels or shoes that don’t fit too well
- If you have a foot deformity (e.g. hammertoes and bunions)
- If you are a heavyweight (extra weight adds extra pressure on the foot)
- If you have high arches or a long second toe
Moreover, as you age, the fat pad that cushions the ball of your foot gets thinner, thereby reducing the support of your metatarsal bones. This can also increase your risk of developing a dropped foot metatarsal.
How is Dropped Metatarsal Diagnosed?
Pain in the foot that lasts for a long time can be caused by medical conditions other than a metatarsal drop, including Achilles tendonitis, arthritis, or a broken toe.
To pinpoint why your foot hurts, your orthopedist or podiatrist will thoroughly examine your foot while you are standing and when you are seated.
You will also be asked about your daily activities, how much time you spend standing up, what type of shoes you wear, and what type of workout you do.
After that, your doctor may request the following imaging techniques:
- An X-Ray to exclude a stress fracture or other foot problems
- A bone scan to locate the point of inflammation
- An ultrasound to rule out other causes of pain in the metatarsal area (e.g. bursitis and Morton’s neuroma)
- An MRI to look for the source of pain in the midfoot area and metatarsal region (e.g. traumatic disorders, circulatory conditions, hammertoe, dropped arches)
Different foot problems can cause symptoms similar to metatarsalgia from a fallen metatarsal arch.
Using the results of the imaging tests and the information gathered, your doctor will be able to make a diagnosis and come up with an effective dropped metatarsal treatment plan.
What is the Treatment For Dropped Metatarsal?
Your foot and ankle doctor will give you instructions on how to manage your dropped metatarsal head and metatarsalgia.
Home remedies
There are many lifestyle adjustments and home remedies that can help relieve your metatarsal pain and inflammation. Try to:
- Not stress your feet to decrease the pressure on your metatarsals
- Use over the counter pain meds to relieve the pain
- Keep your foot elevated/propped up whenever you can
- Avoid wearing shoes that are too tight or too loose
- Apply ice on your foot or roll it over a frozen bottle of water
- Keep your floor clear of things you might accidentally step on and hurt your foot with
- Avoid intense physical activities, especially those that put pressure on the feet
- Perform gentle stretching and strengthening exercises for your foot
Weight management can also help reduce dropped metatarsalgia. When the weight drops, the pressure over the foot also decreases.
Conservative treatment
Your doctor may recommend the following non-surgical ways to treat dropped metatarsal pain and discomfort in your feet:
- Pain medications and anti-inflammatory drugs
- Pressure bandage around the ball of the foot
- Customized orthotic foot inserts (metatarsal pads or arch support) worn inside the shoes to realign the foot and improve its function
- Braces or splints in the shoes to hold your foot in the proper position
- Physical therapy exercises to strengthen the foot muscle, relieve pain, and improve gait problems
Surgical treatment
If conservative treatment doesn't work, your metatarsal foot problem can start to worsen. Moreover, your metatarsalgia may be complicated by other painful foot conditions such as a hammertoe or foot bunions.
In that case, your doctor might recommend a surgery called metatarsal osteotomy to realign the collapsed metatarsal bones into a normal position.
Dropped metatarsal surgery involves cutting the misaligned metatarsal bone behind the toe, properly repositioning it, then holding it in place with a surgical pin or screw.
Conclusion
Metatarsalgia resulting from a dropped metatarsal bone in the foot can become debilitating. If you have unresolved, severe foot pain, consult with your family doctor or general practitioner, who can refer you to a bone or foot specialist.
Proper diagnosis and treatment of fallen metatarsal can relieve your pain, ease your discomfort, and enable you to perform your daily activities unbothered.
To search for the best Orthopedics Healthcare Providers in Croatia, Germany, India, Malaysia, Singapore, Spain, Thailand, Turkey, Ukraine, the UAE, UK and the USA, please use the Mya Care search engine.
Dr. Mersad is a medical doctor, author, and editor based in Germany. He has managed to publish several research papers early in his career. He is passionate about spreading medical knowledge. Thus, he spends a big portion of his time writing educational articles for everyone to learn.
Sources:
Featured Blogs



