Minimally Invasive Mitral Valve Repair Surgery – Benefits Over Conventional Approach
Minimally Invasive Repair vs Conventional Surgery
The mitral valve is one of four valves that control blood flow between the heart chambers. The mitral valve lies between the left atrium and left ventricle, preventing blood from leaking back into the left atrium during ejection (systole).
The normal mitral valve opens when the left ventricle relaxes (diastole), allowing blood from the left atrium to fill the decompressed left ventricle. When the left ventricle contracts (systole), the increase in pressure within the ventricle causes the valve to close, preventing blood from leaking into the left atrium and assuring that all of the blood leaving the left ventricle (the stroke volume) is ejected through the aortic valve into the aorta and to the body.
Signs and symptoms of mitral valve disease can include:
- Fatigue
- Irregular heart sound (heart murmur)
- Irregular heartbeat
- Shortness of breath
The mitral valve can become incompetent in some patients - a condition known as mitral valve regurgitation or mitral valve insufficiency. It is a fairly common condition affecting up to 10% of the population and can potentially lead to heart failure and other maladies if left untreated. A damaged mitral valve may be a congenital defect or caused by degenerative disease.
Degenerative mitral valve disease is a common disorder affecting around 2% of the population.1 The most common finding in patients with degenerative valve disease is leaflet prolapse due to elongation or rupture of the chordal apparatus, resulting in varying degrees of mitral valve regurgitation due to leaflet malcoaptation during ventricular contraction
Traditional mitral valve surgery replaces or repairs the incompetent mitral valve through a large mid-chest opening (Full sternotomy). Minimally invasive mitral valve repair through a much smaller incision is, however, becoming more and more popular. This advanced technique has been shown to lead to better recovery, better results, less trauma, and fewer post-op complications.
What is Mitral Valve Regurgitation?
In a normal healthy heart, the mitral valve is completely closed when the heart pumps, preventing any blood from flowing backwards into the left atrium. If the mitral valve is incompetent for any reason, blood will flow backward through it to the left atrium. This is called mitral regurgitation. A common cause of mitral regurgitation is mitral valve prolapse - where one or both of the leaflets of the mitral valve collapse or bulge backward.
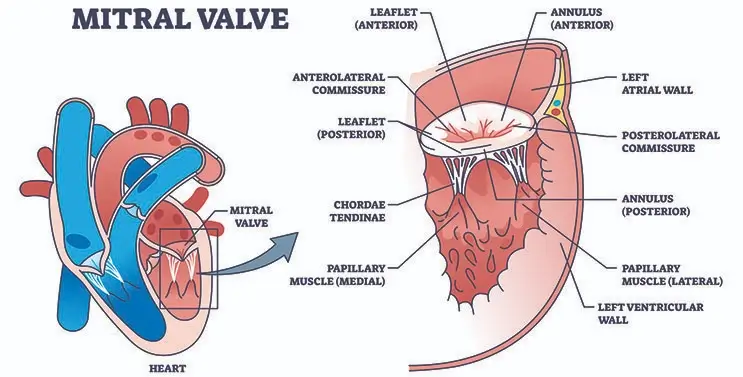
The main components of the mitral apparatus are the mitral annulus, the mitral leaflets, the chordae tendineae, and the papillary muscles. Normal valve function is dependent on the integrity and normal interplay of these components. Abnormal function of any one of the components, or their interplay, can result in mitral regurgitation.
- Annulus - A fibrous ring around the mitral valve. It is dynamic throughout the cardiac cycle, is made out of parallel collagen fibers, and is well-defined histologically. It is non-planar and shaped like a saddle.
- Anterior and posterior leaflets (flaps) - This is the mobile part of the valve.
- Chordae tendineae - Tendinous cords originating from the papillary muscle tips that insert into leaflets.
- Papillary Muscles.
- The atrial and ventricular walls.
When Is Treatment Needed?
Treatment of mitral valve incompetence is not always necessary. Candidates for mitral valve repair might get a recommendation from their surgeon based on the following:
- You have mitral valve regurgitation symptoms (breathlessness, fatigue, lung edema, etc.), or subclinical indicators (left ventricular dilatation or dysfunction)
- You are undergoing cardiac surgery for another reason and have mitral regurgitation too.
- You have high-grade mitral valve regurgitation, even if you don’t have any symptoms.
The decision for mitral valve repair in asymptomatic patients, assessing the risks and benefits of minimally invasive mitral valve repair, is taken on a case-by-case basis. Early mitral valve repair stresses the need for: appropriate echo evaluation, a surgeon with experience in mitral valve repair (Likelihood of successful repair > 95% of cases with mortality < 1%), and an experienced postoperative team (Multidisciplinary and accredited heart valve surgery unit) is advisable.
Mitral Regurgitation Surgery Options
When it comes to mitral valve regurgitation surgery, there are a few options. Top global heart centers offer a full range of mitral valve treatment options, including:
- Traditional Mitral valve replacement or repair: Conventional replacement or repair through a large chest incision (Full sternotomy)
- Minimally invasive Mitral valve repair/replacement: Advanced and minimally-traumatic approach through a much smaller chest incision.
- Transcatheter mitral valve repair/replacement: A newly emerging method done without open-heart surgery.
The choice of surgery usually depends on the patient´s condition, the experience of your surgeon, and the qualifications of the heart center.
Minimally Invasive Repair vs Conventional Mitral Valve Surgery
Minimally invasive repair, when available, is thought to be superior to conventional mitral valve surgery.
Over the years, unique techniques to surgically repair the mitral valve and related structures (e.g. the chordae and papillary muscles), without the need for a heart valve replacement, were developed. This minimally invasive approach involves reconstructing the mitral valve and restoring its competence.
The minimally invasive approach is much less traumatic than the conventional mid-chest approach. In minimally invasive mitral valve surgery, a small 4-6 cm right posterolateral incision is made between the ribs (no bone cutting). In the traditional approach, the breast bone (sternum) is vertically cut in the medium line, with a 15-20 cm long incision - a very traumatic approach.
In addition to causing less trauma, minimally invasive mitral valve surgery has been shown to have many advantages over traditional open surgery.
Benefits of Minimally Invasive Mitral Valve Surgery
Minimally invasive mitral valve repair is a hot topic of research in the field of cardiac surgery. So far, studies at prominent centers around the world have found several advantages of minimally invasive valvuloplasty over conventional methods:
- Faster recovery timeline
- Shorter stay at the hospital
- Earlier mobilization of patients
- Less need for blood transfusion
- Less pain
- Less risk of post-op heart rhythm problems
- Less risk of post-op wound infection
- Better long term survival
- Better heart function outcomes
- Lower risk of blood clots after surgery
Despite the clear benefits of minimally invasive mitral valve repair, its availability is still limited to heart surgery centers of excellence due to the complexity of the surgery and the needed surgical skills.
How is Minimally Invasive Mitral Valve Surgery Performed?
Minimally invasive mitral valve surgery is done under general anesthesia. You are completely put to sleep and won’t feel anything.
The surgeon will then perform a 4-6 cm skin incision in the right posterolateral chest zone between the 4th and 5th ribs. The ribs will be pulled apart using a special retractor to expose the heart.
The lungs and heart will be stopped at this stage, and you will receive all your oxygen needs from a machine connected to your femoral (groin) vessels called an extracorporeal circulation or heart-lung machine.
The valve repair then commences using specialized surgical instruments designed specifically for minimally invasive heart surgery. The surgical repair or replacement of a heart valve depends on the individual valve pathology. The surgeon might reinforce the valve (annuloplasty), replace it, remove or reimplant the chordae and papillary muscles, repair the leaflets, or do a combination of all these.
After surgery, you will be taken to the cardiac care unit for close monitoring.
Is Minimally Invasive Mitral Surgery an Option For You?
The minimally invasive mitral repair approach is widely regarded as the best method available today to treat mitral regurgitation. To know whether you are a candidate for minimally invasive heart surgery, a team of cardiologists and cardiac surgeons needs to individually assess your case.
Radiologic, echocardiographic, and laboratory tests will be ordered to identify mitral valve problems and determine if a minimally invasive repair can be successfully done.
If minimally invasive mitral repair is a viable option, you will be planned for surgical pre-op clearance and given full instructions on how you and your care team can prepare together for surgery.

Dr. Xavier Ruyra is the Director of the Heart Surgery Program at Teknon Medical Center (Quirónsalud) in Barcelona, Spain, and President of the CardioDreams Foundation. He is one of the top experts in Valve Repair and the Ross procedure, thus preventing their replacement with artificial prosthetics and reconstructive surgery of the heart chambers. Dr. Ruyra is a specialist in minimally invasive heart surgery and bloodless heart surgery and has developed multiple surgical techniques that are minimally damaging to the patient’s heart. He is also the creator of the "Smart Cardiac Surgery Program" which aims to deliver training courses to produce exceptionally skilled cardiac surgeons. He combines his work as a surgeon with teaching at the University of Barcelona, where he is an Associate Cardiac Surgery Professor. He has published 65 articles in specialized journals and 3 chapters of books. He has also participated in more than 300 national & international conferences and seminars and has developed several patents for devices used for valve repair or reconstruction.

Teknon Medical Center (Quirónsalud) is one of the leading private sector hospitals in Spain, delivering high-quality medical care with personal attention and utilizing the latest technologies. Led by Dr. Xavier Ruyra, the cardiac surgery unit based in the Teknon Medical Center in Barcelona has performed open-heart surgery, minimally invasive, and transcatheter procedures on more than 10,000 patients with outstanding outcomes. During this time, the group introduced the very latest in cardiac surgery technology, developing innovative surgical techniques. Their efforts achieved both national and international recognition for excellent results, compassionate patient care, superior outcomes, and state-of-the-art cardiac therapies.
For more details, please visit https://www.quironsalud-hospitals.com/
Sources:
Featured Blogs



