Surgical Management of Nerve Disorders: A Multidisciplinary Approach
A general perception is that there is no way to improve severe nerve injury or its effect on the limbs. Patients with nerve disorders, neuropathic pain, spasticity, or tetraplegia suffer from poor functions in their extremities. Simple tasks such as grabbing a cup, brushing teeth, or getting into bed can seem impossible to them. Studies reveal that peripheral nerve disorders affect approximately 2.4% of the global population, with the prevalence increasing to 8% among the elderly.
This article explores the latest surgical procedures utilized at top global hospitals to treat nerve disorders.
Innovative Approaches to Treat Nerve Injury
Historically, there have been two surgical approaches to treat patients with nerve disorders; nerve grafts or neurolysis. Since then, newer techniques have been developed to help the nerves regrow and restore function to the muscles:
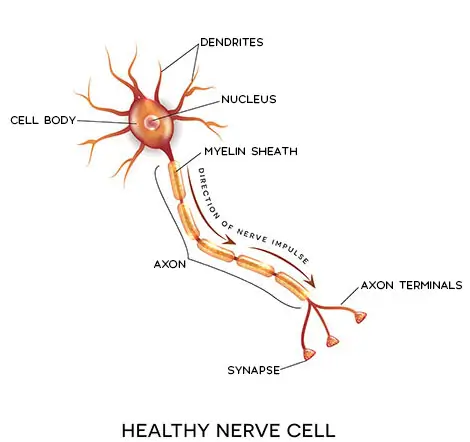
Nerve Transfer
A nerve graft is usually used when the nerve injury is far away from the muscle controlled by the nerve. However, nerve grafts need a very long time to heal. This can lead to poor nerve regeneration and mediocre results. A nerve transfer, on the other hand, can help overcome that obstacle.
Nerve transfer is a procedure developed to restore function to injured nerves. During a nerve transfer, surgeons re-route a healthy passing nerve to reinnervate the nearby damaged nerve.
This allows the damaged nerve axon to regenerate and resume its function in carrying signals to the muscle and skin.
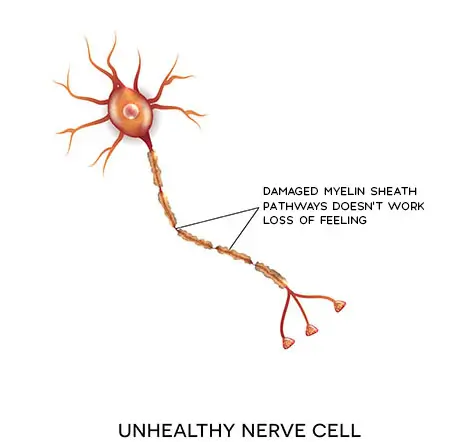
Who can benefit from nerve transfer?
Nerve transfer is the preferred nerve repair approach when:
- The muscle is far from the damaged nerve that supplies it
- A long segment of the nerve is injured
- Your nerve injury is old and has scarring, so you can not benefit from other repair methods like nerve grafts
- The injured nerve is unlikely to regenerate
- You are suffering from a spinal cord injury
The sooner the nerve transfer is performed, the better the chances of saving the muscle from atrophy. Nerve repair should be attempted as soon as possible when unsatisfactory nerve sprouting is detected. There is no particular timeline within which nerve repair is likely to be unsuccessful because several conditions are involved (age, genetics, other illness, concomitant damage, etc). So, consulting a peripheral nerve surgeon for accurate evaluation within 12 months is mandatory to avoid irreversible muscle atrophy.
Supercharged Nerve Transfer
Another nerve repairing technique that was recently developed is the supercharge transfer.
During supercharge nerve transfer, one end of a donor nerve is brought closer together with the side of the damaged recipient nerve. This creates a shortcut to the injured nerve, allowing it to heal faster and better.
Who can benefit from supercharge nerve transfer?
The supercharge nerve transfer approach may be recommended in the following scenarios:
- In 2nd/3rd-degree nerve injury cases
- Poor or light nerve recovery (spontaneous or repaired) to improve motor recovery
- To improve the function of the shoulder, elbow, wrist and hand weakened by damaged nerves
Nerve Allograft
A technique to repair nerves that was developed in the past 15 years is the use of allograft.
During an allograft, a nerve segment is taken from a donor (deceased) and surgically sutured to the injured nerve to cover nerve gaps or for treatment of neuropathic pain. Using frozen nerves harvested from cadavers offers the following advantages:
- It reduces the morbidity risk of harvesting nerves from the patient’s own body
- It offers more stock to be able to reconstruct nerve defects properly
Who can benefit from nerve allograft?
Nerve allografts offer alternatives to autologous nerve grafting when:
- The nerve injury has a larger gap that needs to be bridged
- The nerve injury has a large diameter
- A larger number of donor nerves is needed
- Treatment of selected and considerable amount of cases of neuropathic pain. Such cases include terminal painful neuroma or painful neuroma in continuity
Intraoperative Nerve conduction studies
In the 21st century, nerve surgery primarily relies on intraoperative nerve conduction studies. Several techniques are used to evaluate roots and nerves in adults and babies.
NERVE AND ROOTS
- Nerve Action Potential (NAP): Nerve to nerve conduction
- Compound Muscle Action Potential (cMAP): Nerve to muscle conduction
- Sensory nerve conduction (SNC)
ROOTS
- Somato Sensory Evoked Potentials (SSEP)
- Motor Evoked Potentials (MEP)
Satisfactory and successful surgical results in obstetrical and adult brachial plexus injuries, peripheral nerve damage, and tetraplagia depend on:
- High-level surgical expertise in diagnosis and experience in managing technique-based options
- Use of intraopertive nerve recording by a neurologist
- Multidisciplinary and trained approach
Tendon transfer
When the treatment of an injured nerve is delayed or failed, surgical nerve repair may no longer be an option. Often, the damage is permanent, and muscle function is lost. In these cases, since the nerves cannot be repaired, surgeons might recommend tendon transfer surgery.
Tendon transfer surgery is when a tendon from a nearby well-innervated muscle is re-routed and attached to the paralyzed muscle. This will restore muscle control and improve mobility and motion.
Who can benefit from tendon transfer surgery?
- All cases lacking some degree of nerve function with preserved agonistic or antagonistic tendon/muscular function at the same extremity
- Patients with severe chronic damage to the hand nerves (median and/or ulnar nerves)
- Patients with injuries to the upper extremities
- Patients with hand, arm, or leg palsy
Nerve Injuries that Require Surgery
Worldwide, only a few hospitals have expertise with a combination of modern approaches to treat nerve injuries. Some of the complex nerve injuries that could be successfully treated include:
- Brachial plexus Injury: The nerves in your shoulders, arms, or hands can become damaged after a car accident (bike, car, snowmobile) or a fall. You might lose strength in your arm, or it can even become paralyzed. In each case, surgeons use a combination of multiple techniques such as nerve graft, neurolysis and nerve transfers to treat brachial plexus injury and restore muscle functions.
- Isolated nerve injury: Excessive stress on the shoulder from extreme sports or an injury can damage some shoulder nerves. Top centers offer a full spectrum of nerve repair techniques to diagnose and treat isolated shoulder nerve injuries.
- Neuropathic pain: Pain management plays a vital role in recovery. Even when patients have good muscle recovery, they wouldn’t be able to move their muscles properly because of neuropathic pain. Advanced neuroorthopedics centers offer the most advanced methods to evaluate the source of neuropathic pain, such as Microneurography, Peripheral Nerve Excitability, Electromyography and Nerve Conduction Studies, Somatosensory Evoked Potentials – Conventional SSEP, Laser Evoked Potentials (LEP), Contact Heat Evoked Potentials (CHEPS), and Quantitative Sensory Testing. Surgeons then decide on the best option to improve muscle function by surgically relieving the source of pain.
- Spasticity: After brain trauma or a stroke, the arm, shoulder, elbow, or wrist can become spastic. This abnormal contraction of the muscles causes pain, poor muscle function, hygiene concerns, and cosmetic problems. By combining different nerve treatment approaches, patients gain improved muscle function, improved posture, and more independence to perform certain tasks on their own.
- Tetraplegia: In the cases where there is severe spinal cord damage, it is important to be able to restore (at least) some essential motor functions. Combining different techniques such as tendon transfer, nerve transfer, and joint release can restore elbow extension in paralyzed patients. This makes it easier for tetraplegic patients to get on their wheelchair, transfer to bed, or extend their hand in space to grab things.
Managing complex neuroorthopedic injuries requires ample experience and highly qualified expertise to know which technique or combination of techniques to use for surgically restoring nerve function and mobility from nerve damage.
Combined Treatments
Often, a combination of different techniques give patients the best results possible. Depending on the injury and the lost motor functions, the following techniques can be used in combination:
- Tendon transfer
- Joint release
- Joint Fusion
- Botulinum toxin therapy
- Osteotomy
- Denervation
- Hyponeurotization (a recently used technique that releases the muscle from a spastic nerve)
- Tendon release
By using a combination of different nerve repair techniques, patients can regain muscle function and control in a one step surgery.

Dr. Joaquim Casañas heads the Trauma Unit of the Traumatology and Orthopedic Surgery Unit at the Centro Médico Teknon Grupo Quirónsalud AKA Teknon Medical Center in Barcelona, Spain. Dr. Casañas is a renowned specialist in peripheral nerve and hand surgery, devoting himself exclusively to the diagnosis and treatment of diseases of the hand and upper limbs. Exceptionally qualified in his field, he holds a Diploma in Integrated Health Systems ESADE (Health Management) and Hand Surgery from the Federation of European Societies.

Led by Dr. Casanas, the Teknon Medical Center in Barcelona is one of the top hand surgery referral centers in Spain, Europe, and the world. The specialized unit offers a multidisciplinary approach to peripheral nerve surgery that is not available in many other places in the world. The center brings together a team of hand therapists, neurologists, intraoperative neurophysiologists, and pain specialists. The team deals with complex nerve injuries using cutting-edge medical technology. Surgeons perform advanced surgical approaches including nerve transfer, supercharge transfer, allograft, and tendon transfer to treat nerve injuries and restore muscle function.
For more details, please visit https://www.quironsalud-hospitals.com/
Sources:
Featured Blogs



