Temporomandibular Disorders: Causes, Symptoms, Diagnosis, and Treatment

The temporomandibular joint assists in the trouble-free opening, closing, and side to side movements of the mouth. Whenever individuals yawn, talk or chew food, they are using the temporomandibular joint (TMJ). Various conditions may affect the joint and cause jaw pain and other associated symptoms. These symptoms significantly affect the quality of life of affected individuals.
In this article, we discuss temporomandibular joint disorders, their symptoms, causes, and management.
Location of the Temporomandibular Joint (TMJ)
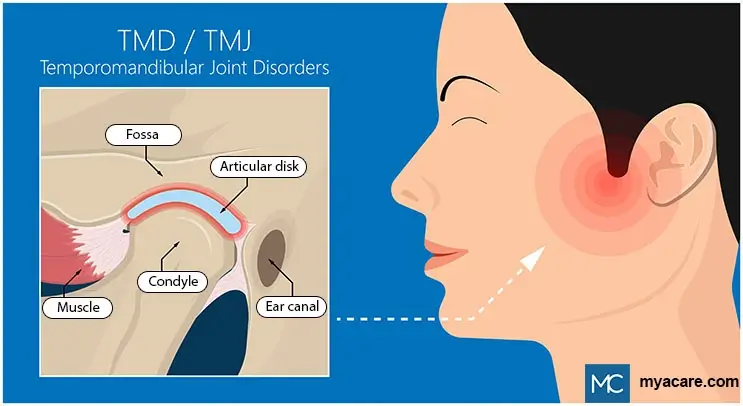
TMJ is present on each side of the head in front of the ears and connects the lower jaw to the skull (near the temple). It is composed of a rounded protrusion (condyle) of the lower jaw that sits into the indentation (socket-like space) in the skull. TMJ contains an articular disk which is a soft disc-like structure that serves as a cushion and enables smooth movement of the jaw.
What are Temporomandibular Joint Disorders?
The temporomandibular joint disorder is a group of conditions that cause dysfunction in the joints and muscles that control jaw movements. It causes chronic pain of non-dental origin in the oral or facial region. It affects 10-15% of people globally. However, only 5% seek treatment. Temporomandibular disorders are more commonly found in the age group of 20-40-year-olds and affect more women than men.
What are the Causes of Temporomandibular Disorders?
The exact cause of TMJ disorders is unknown. However, temporomandibular disorders are either due to pain in the muscles around TMJ that control jaw movement or problems in the joint.
Here are some of the conditions that cause pain in the TMJ muscles
- Misalignment of teeth
- Abnormal bite between teeth
- Parafunctional habits such as teeth grinding or teeth clenching
- Stress and anxiety
- Abnormal displacement of the articular disk (a soft disc-like structure present between the TMJ joint)
Here are some of the conditions that cause pain in the temporomandibular joint
- Trauma or injury to the joint
- Degenerative changes such as osteoarthritis, ankylosis (stiffness due to fusion of bones that form TMJ)
- Displacement or dislocation of the joint (Occurs when condyle displaces out of the socket space)
- Tumors in the TMJ
- Abnormal development of joint from birth
What are the Symptoms of Temporomandibular Disorders?
Here are some of the symptoms of temporomandibular disorders:
- Pain in joint or surrounding areas: Individuals may experience pain in front of the ear which may spread to surrounding areas such as ears, cheeks, teeth, forehead, and neck. Pain may be present either on one side or both sides during rest or while talking, yawning, or chewing food.
- Clicking, grinding, or popping sounds: Clicking sounds can be heard from the TMJ when an individual makes jaw movements while chewing food, opening, or closing their mouth. Clicking or popping sound is due to abnormal shifting of the articular disk from its original position inside the joint.
- Reduced mouth opening: Individuals may develop a feeling of tightness in the jaws or may experience jaw getting stuck frequently. In some instances, individuals may develop lockjaw, affecting jaw movements.
- Discomfort in the ears: Due to the proximity of ears to TMJ, individuals with temporomandibular disorders may experience noise in the ear, vertigo (dizziness), and sensitivity to sound.
- Headaches: Individuals often experience dull headaches (mostly in the mornings). Involuntary teeth clenching or teeth grinding during sleep causes pain in the TMJ muscles. Since the muscles are present along the head and face, they result in headaches and facial pain.
How are Temporomandibular Disorders Diagnosed?
A dentist can help identify temporomandibular disorders with the help of clinical and radiographic examinations.
Clinical Examination:
The dentist will discuss the individual’s medical history and discuss the symptoms. Presence of most common symptoms such as pain in the jaw, headache, neck pain, restricted mouth opening, and clicking sounds while opening or closing of jaws may indicate the presence of temporomandibular disorders. Further, the dentist will place his/her finger and feel the TMJ joint and nearby muscles to locate the site of pain. He/she may place the finger over the TMJ or inside the ear canal and ask the patient to open and close the mouth. This helps determine the presence of a clicking sound. Presence of a clicking sound is considered normal if not associated with symptoms such as pain and restricted mouth opening. Pain and swelling in the TMJ region indicate the presence of inflammation.
Radiographic Examination:
- Conventional X rays (Panoramic radiographs): Conventional X rays give an overview of jaws and teeth. These X rays also help in the evaluation of symmetries of the jaws, abnormality in the teeth and maxillary sinus disease, and fractures of the condyle. This technique is used for screening the condition. The presence of disease is confirmed with more advanced radiographic techniques.
- CT scans (Computed Tomography): CT scans help evaluate the presence of ankylosis (stiffness) in the joint, tumors, abnormal bone growth, and erosion of the joint.
- MRI (Magnetic Resonance Imaging): This non-invasive technique helps assess soft tissues of the joint such as the articular disk, muscles around TMJ, and swelling around the joint.
- Arthrography: In arthrography, a radiopaque contrast agent is injected into the joint region, and radiographs are taken. This technique helps in the assessment of perforations in the articular disk and muscles around the joint.
What are the Treatment Options for Temporomandibular Disorders?
Temporomandibular disorders are considered self-limiting. Many patients experience improvement in the signs and symptoms without any treatment. However, non-invasive treatments are considered helpful in individuals who require treatment. In rare cases, surgical intervention is required.
Non-invasive therapy:
- Medications: Intake of painkillers and muscle relaxants help reduce pain and muscle spasm (strain) respectively. In some cases, antidepressants may be used to treat chronic TMJ disorders due to continuous grinding or clenching of teeth.
- Jaw exercises: Jaw exercises such as guided opening and closing of the mouth, and gentle tension exercises against resistance improve the strength of TMJ muscles.
- Injections: Local anesthesia or steroids can be used to treat the inflammation or swelling in the joint. Local anesthesia also helps in treating chronic grinding of teeth (bruxism).
- Correction of dental occlusion: Placement of dental splints or nightguards (retainer-like plastic piece) and permanent correction of misaligned teeth may help in treating TMJ disorders.
- Manual reduction in cases of sudden disk displacement: Sometimes, the individual may experience lockjaw while opening the mouth wide. In such instances, lockjaw can be corrected by inserting both thumbs into the patient’s mouth (on the upper surfaces of lower teeth) and fingers grasping under the chin. Thumbs are used to push down the posterior teeth and fingers to pull up the chin. This allows the repositioning of the articular disk into its original place.
- Psychological counseling: In case of stress and anxiety, a psychiatrist consultation is recommended, who may introduce the individual to stress coping skills and relaxation techniques.
- Surgery: In individuals with the presence of tumors, fractures, congenital disorders, and ankylosis, a surgery is recommended to restore the normal function of the joint.
How to Manage Symptoms of Temporomandibular Disorders at Home?
Symptoms of TMJ disorders can be managed at home through the following activities:
- Eat soft food
- Avoid chewing gum and sticky chocolates
- Practice jaw exercises, meditation, and relaxation techniques
- Avoid wide opening of mouth for yawning, chewing, or talking
- Apply heat packs intermittently at the site of discomfort
- Take medicines on time as prescribed
- Place a nightguard on teeth before sleeping at night
- Avoid biting of nails
To search for the best dentists in Germany, India, Malaysia, Poland, Singapore, Spain, Thailand, Turkey, the UAE, the UK and the USA, please use the Mya Care search engine.
To search for the best healthcare providers worldwide, please use the Mya Care search engine.

Dr. Shilpy Bhandari is an experienced dental surgeon, with specialization in periodontics and implantology. She received her graduate and postgraduate education from Rajiv Gandhi University of Health Sciences in India. Besides her private practice, she enjoys writing on medical topics. She is also interested in evidence-based academic writing and has published several articles in international journals.
References:
Featured Blogs



