10 Ways to Save a Diabetic Foot From Amputation

Diabetic foot ulcer is a serious complication of diabetes mellitus. It can lead to amputation and disability. That’s why doctors are now so focused on diabetic foot ulcer treatment and preservation to prevent amputation.
Worldwide Statistics from the American Diabetes Association state that a person loses a limb due to diabetes-related complications every 30 seconds. According to a 2019 Statista report, Germany had the highest prevalence of diabetes in Europe among their adult population with 15.3 percent living with diabetes. Furthermore, it is estimated that about 15% of seven million people with diabetes mellitus in Germany suffer from Diabetic Foot Syndrome (DFS). Alarmingly, studies reveal that almost 50% of patients with Diabetic Foot Syndrome (DFS) have had major or minor amputations.
Luckily foot ulcers, diabetic foot, leg, toe, or foot amputation are all preventable. For instance, regular foot examinations could reduce the risk of amputation significantly.
From proper foot care to regular foot checkups, there are many things you can do to keep healthy feet despite diabetes.
What Is Diabetic Foot?
Diabetic foot is one of the feared complications of diabetes.
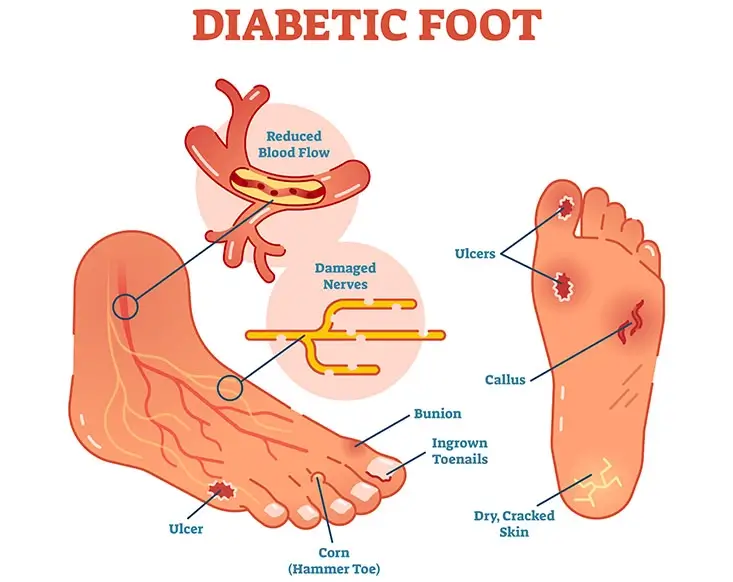
Chronic high blood sugar leads to blood vessel damage. This includes blood vessels that provide the nerves in your toes, feet, and legs with oxygen and nutrients.
Having uncontrolled diabetes for a long time will damage the nerves in your legs. Damaged nerves lead to a reduction or loss of sensation in the feet. So, if you wound your leg in any way, you might not feel it until it’s too late.
To make things more complicated, wounds tend to heal slower in people with diabetes since blood vessels can’t properly deliver blood.
All of these together can lead to a foot ulcer - an open non-healing foot wound. And, if an ulcer is not treated in time, it can become infected. There is also the risk of the infection spreading to the bone, leaving foot amputation as the sole treatment option.
Why Do Diabetics Sometimes Need Amputation?
Not every foot ulcer needs an amputation. We doctors do our best to prevent amputation and preserve the toes, feet, and legs of all patients.
However, when a diabetic foot ulcer fails to heal or becomes necrotic (has dead tissue), gets infected, or spreads to deeper tissue, then amputation might be the only treatment choice.
Diabetic foot amputation, when necessary, will prevent the spread of infection to the bloodstream (sepsis) - a dramatic and fatal complication in many cases.
But it’s not all grim. There’s a lot you can do to stop this before it even happens.
10 Ways to Save a Diabetic Foot from Amputation
1. Always Check Your Feet
Your podiatrist or endocrinologist has probably already told you that you should regularly inspect your feet. Even the smallest cut wound can lead to a diabetic foot ulcer and progressively worsen and require amputation.
Diabetic neuropathy makes you lose sensation in your feet. Regular foot inspection is - without a doubt- the best way to prevent diabetic foot and amputation.
Cracks, blisters, cuts, growths, sores, and wounds should all be reported to your healthcare provider. Take your time when inspecting your foot, and carefully check between your toes.
You can use a magnifying glass if your vision is poor. You can ask your caregiver to check your feet for you if you’re unable to do it yourself.
2. Keep Your Feet Clean
If you have diabetes, washing your feet daily can help prevent foot amputation. Foot hygiene is an essential part of diabetic foot preservation.
Make sure to wash your feet with warm water. Not too hot, not too cold. Rub your feet gently using non-irritating soap. Once done, gently tap them dry, especially between the toes. Make sure not to rub too hard as this might cause the skin to break.
3. Don’t Attempt to Remove Foot Lesions Yourself
No matter how tempting it gets, you cannot remove any growths, lesions, or plaques off your foot yourself.
Only a specialist foot surgeon should perform even the most minor procedures to prevent complications.
Whether it’s a callus, wart, or bunion, removing a foot skin lesion yourself in a non-sterile technique can lead to infection. A non-healing foot wound (ulcer) can form. And if the infection spreads to the bone, surgical debridement, and toe, foot, or leg amputation might not be avoidable.
4. Be Careful When Cutting Your Toenails
When cutting your toenails, cut only your toenails. Don’t try to cut any skin, even if it looks dead and dry.
You should be careful when trimming your toenails so that you don’t cause any accidental injuries. Remember, pain sensation in the feet is decreased in people with diabetes.
You’d be surprised to learn that simple toenail trimming can be a risk factor for amputation. Taking your time and doing it carefully is essential for diabetic foot ulcer prevention.
5. Protect Your Feet
Never go barefoot. Even at home.
Although it might sound perfectly safe, you should never walk barefoot if you have diabetes. You’d be risking too much. As a diabetic, you need to keep in mind that a foot ulcer can develop from the smallest of wounds. A tiny crack can lead to amputation if not handled in time.
So, how about you take an extra 10 seconds to put your slippers on next time you’re walking around the house?
6. Have a Proper Foot Routine
If you want healthy feet, and want to prevent diabetic foot amputation, then you might want to go the extra mile.
In addition to regularly washing your feet, consider using a moisturizer, powder, and special protective products to keep the skin moist and smooth.
7. Don’t Wear Shoes That Don’t Fit
No matter how good they look, if a pair of shoes is squeezing on your feet, give it away.
Wearing tight shoes can push your toes together, causing skin injuries, and possibly leading to diabetic foot ulcers.
8. Stop Smoking
Smoking is an independent risk factor for peripheral arterial disease. As long as you smoke, your wound-healing ability is decreased. Not enough oxygen and nutrients would reach your wound.
If you are serious about preventing foot ulcers and diabetic amputation, then consider quitting smoking for good.
9. Keep Your Blood Sugar in Check
Chronically high blood sugar reduces your immunity, speeds up the progression of complications, and reduces your wound healing ability.
Make sure your blood sugar levels are always under control. Take your medications as prescribed. If you still have high blood sugar, make an appointment with your endocrinologist to re-evaluate your care plan.
10. Always Check with a Foot Specialist
You should see a foot specialist (podiatrist) or a foot surgeon at least once a year to have your feet checked.
Your healthcare provider will carefully inspect your feet, ask you about your routine, and make further recommendations regarding foot care. Getting regular checkups is essential to diagnose foot ulcers early and have them treated in time - before they lead to amputation.
The 4 Stage Therapy Concept
For those with diabetic foot ulcers and resultant foot deformity, the 4 Stage Therapy Concept has shown good outcomes. According to the statistics, the successful progression of treatment to the 4th stage minimizes the risk of amputation to close to 1%.
To learn more please see the following article.
Outlook
Not every diabetic patient ends up with an amputation. If you take good care of your feet, follow up regularly with a foot specialist, and lead a healthy lifestyle, then foot amputation can be prevented.
Taking a few extra minutes a day to make sure everything is in order will prove worth it in time.

Prof. Dr. med. Martinus Richter is Head of the Department for Foot and Ankle Surgery at the Rummelsberg Hospital in Schwarzenbruck, Germany. He is a specialist in orthopedics and trauma surgery, sports medicine, and a certified foot surgeon (certified by the German Society for Orthopedics and Trauma Surgery). Prof. Martinus Richter has served as president of organizations such as International Federation of Foot and Ankle Societies (IFFAS), European Foot and Ankle Society (EFAS), and International WBCT Society.
Sources:
Featured Blogs

Medically Induced Coma: What It Is, How It Works, Who Benefits, and Recovery Outcomes


