4-Stage Therapy Concept – Avoid Amputation Due to Diabetic Foot
Diabetes is the number one cause of foot amputation worldwide. In Germany alone, more than 50,000 foot amputations are performed each year. Patients are left with a physical disability which often leads to a restricted lifestyle and reduced quality of life. Fortunately, reports indicate that a team-based approach incorporating improved screening, prevention programs focusing on how to care for diabetic feet, and early interventions to manage diabetic foot ulcers can reduce long-term amputation rates significantly.
This is why doctors emphasize the importance of foot preservation to prevent diabetic foot amputation. In this article, we look at an evidence-based 4-Stage Therapy Concept that aims to fix diabetic foot deformity and prevent future ulceration that might lead to infection and amputation.
This protocol has been extensively studied and has shown a significant reduction in the need for amputation. The rationale is to treat the deformity that causes ulcers to develop, effectively preserving the foot and protecting it from future injury. Based on published research of over 250 cases, a very low rate of major amputation (lower leg level) of 1.3% was reported.
What Is Diabetic Foot Deformity?
Diabetes is a very common metabolic illness that causes your blood sugar to be constantly high. It affects nearly 1 in every 10 individuals, and the prevalence increases with age.
Having high levels of blood sugar for a long time can be very damaging to our bodies. One of the main complications of diabetes is blood vessel damage. The high blood levels slowly destroy tiny blood vessels and cause them to narrow down and sometimes close off completely.
This, in turn, leads to nerve damage, since nerves need oxygen and nutrients from blood circulation. Nerve damage occurs first in the extremities, so patients start to lose sensation first in the feet - a condition called diabetic neuropathy.
This decrease in sensation in the feet prevents patients from feeling pain from foot injuries, abnormal posture, or external physical pressure, and hinders their ability to take normal steps since they don’t get any feedback sensation.
This long-term abnormal weight distribution exerts pressure on the foot bones and joints, leading to misshapen feet - known as diabetic foot deformity.
Why Is Amputation Sometimes Needed?
Often, a small foot wound in diabetics (called a “diabetic ulcer”) can become infected with microbes. If the infection eats into the foot and reaches the bone, the only way to prevent blood poisoning might be foot amputation.
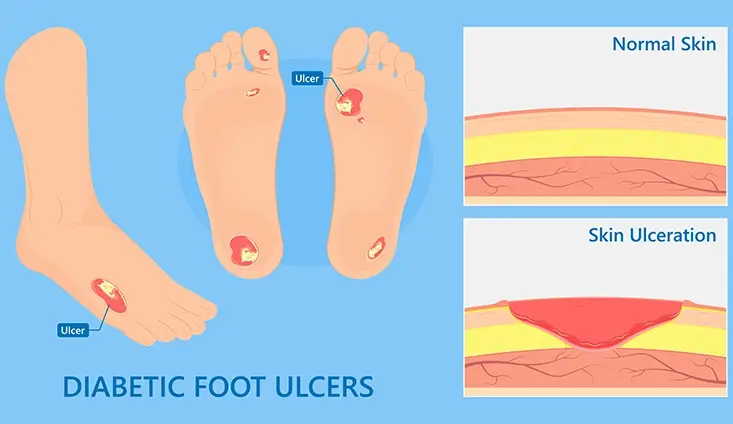
Several factors may lead to the development of foot ulcers:
- Diabetic foot deformity: the abnormal weight distribution on a deformed diabetic foot exerts excessive pressure on the foot skin. This further blocks the blood circulation, causes the skin to break and leads to the formation of diabetic foot ulcers. By fixing diabetic foot deformity, the original cause of diabetic foot ulcers can be treated.
- Decreased blood supply: A chronic complication of diabetes, which reduces wound healing ability.
- Decreased sensation: Due to diabetic neuropathy, if a diabetic person develops a wound, it may go unnoticed since the pain sensation is decreased.
The 4-step protocol goes to the root cause that leads to amputation. By fixing the orthopedic foot deformities caused by diabetes, the weight distribution on the feet will be normalized, preventing future injuries and ulcers.
The 4-Step Diabetic Foot Preservation Plan
A new, innovative 4-step management plan to treat diabetic foot ulcers and significantly reduce the risk of amputation has shown great promise. The end goal of the diabetic foot treatment protocol is to fix the deformity leading to foot ulcers and infection.
The 4-step plan goes like this:
Step 1: Treating the active problem. If you have an ulcer, infected or not, it will be treated with surgical debridement and antibiotics. Debridement means that the wound will be surgically cleaned to allow new vascularized tissue to form. This might be done up to 5 times, in weekly intervals, until the wound is 100% sterile. After the surgery, the wound will be covered with a vacuum dressing.
Step 2: The diabetic foot wound will be closed using sutures or a skin graft if needed
Step 3: Recovery phase - During this time, you will be asked to keep pressure off the wound. This means that you will have to use crutches, walking aids, or specialized shoes to preserve maximal blood flow to the wound.
Step 4: This is the most critical step to preserve the foot, prevent future ulcers, and avoid future amputation. The 4th step includes corrective orthopedic surgery to fix the diabetic foot. The surgery restores the normal curvature of the foot and re-aligns the bones (metatarsals) into a normal orientation.
A deformity can potentially cause the recurrence of an ulcer, hence, correction becomes a crucial aspect of the protocol. The corrective surgery utilizes med-tech advancements such as computer navigation, intraoperative computed tomography, and intraoperative pedography.
The main goal of corrective surgery is a plantigrade (walking with the toes and metatarsals flat on the ground) foot achieving even power distribution and full resilience. Apart from achieving mobilization, which is also important for healthy metabolism in Diabetics, the recurrence of an ulcer is also prevented.
This 4-step plan is both curative and preventive. In the first 3 steps, any active wounds and infections are treated to stop the spread of necrosis and preserve the rest of the foot. In the 4th and most important step, the foot deformity is fixed to normalize the weight distribution on the foot and prevent future pressure ulcers from forming.
Innovative Diabetic Foot Diagnostics
The protocol incorporates innovative and cutting-edge diagnostic equipment, which include:
- Intraoperative Pedography: Allows surgeons to take radiographic images of the foot during the surgery
- 3-D Standing X-rays (with applied stress): Also known as a Digital Volume Tomography using pedCAT. This is one of the most important diagnostic tools in our clinic. It allows us to take radiographic images of the foot while the patient is standing, and stress is applied to the feet. This emphasizes the foot architecture and allows our surgeons to know exactly what needs to be done.
- Computer-assisted Deformity Analysis and Correction: Advanced computer software, such as mediCAD® and Orthoplanner®, allows us to plan surgical correction and implant positioning precisely before going into surgery.
Summary
The treatment of Diabetic Foot encompasses aspects such as foot preservation, timely screening and prevention, and earlier intervention to minimize the need for amputation. Due to the comprehensive nature of care required, a certified center that offers maximal care could offer optimal results. Choosing a doctor, team, and healthcare provider with considerable experience in managing diabetic foot deformity, treating complications, and preventing amputation is of utmost importance.
Highly specialized centers utilize top-of-the-line innovative diagnostic and therapeutic tools to treat diabetic foot deformity and prevent amputation. These centers also employ the most recent evidence-based techniques to maximize therapeutic results and minimize surgical complications.
If you have diabetes, it’s crucial to practice proper foot care on a daily basis and report any problems to your healthcare provider promptly. In the right hands and with early treatment, deformity, the need for hospitalization, and amputation can all be prevented.

Prof. Dr. med. Martinus Richter is the Chief Physician at the Clinic for Foot and Ankle Surgery at the Rummelsberg Hospital in Schwarzenbruck, Germany. He is a specialist in orthopedics and trauma surgery, sports medicine, and a certified foot surgeon (certified by the German Society for Orthopedics and Trauma Surgery). He has served as president of organizations such as International Federation of Foot and Ankle Societies (IFFAS), European Foot and Ankle Society (EFAS), and International WBCT Society.
Sana’s Foot and Ankle Surgery Center
Sana’s Foot and Ankle Surgery Center was the first-ever maximal care center in Germany to be certified in this field. Our center and team are regarded as pioneers in managing diabetic foot deformity, treating complications, and preventing amputation.
The Focus Clinic List 2021 has ranked Sana’s Foot and Ankle Surgery Center among the seven top-tier centers in this field.
The clinic is equipped with top-of-the-line innovative diagnostic and therapeutic tools found only in highly specialized centers. Our Chief Surgeon, Dr. Martinus Richter, has developed a world-renowned 4-step plan to treat diabetic foot deformity and prevent amputation. He and his team implement the most recent evidence-based techniques to maximize therapeutic results and minimize surgical complications.
Our team is always glad to answer your questions and plan your therapeutic journey, no matter where you’re located. Contact us to learn more about how we can help.
Sources:
Featured Blogs

Medically Induced Coma: What It Is, How It Works, Who Benefits, and Recovery Outcomes


