Risky Blood Clots – Learn When Blood Thinners Are Useful
Why and When Blood Thinners are Prescribed or Used
The Benefits of Blood Thinners
The Disadvantages of Blood Thinners
Preventing Problems While on Blood Thinners
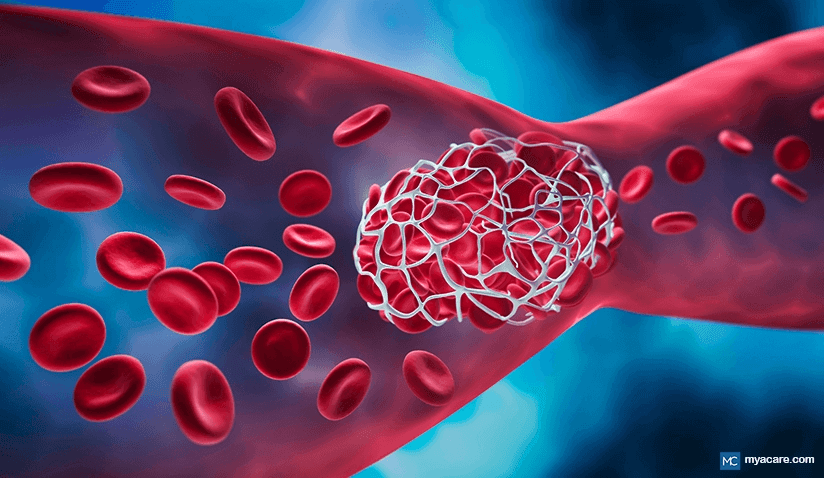
Blood thinners are medications that prevent or reduce the ability of clots to form in the blood. Blood clotting is important when an injury occurs, but when clots form too often or in the wrong place, it can cause major problems such as heart attacks and strokes. Blood thinners may be prescribed to help prevent the formation of problematic clots in the body. According to the CDC, blood clots claim 100,000 lives yearly in the US, with elevated mortality risk in pregnancy and cancers.
How Blood Clotting Occurs
Blood clots are supposed to form when a blood vessel is injured and bleeding. The basic process of blood clotting is outlined below.
- The first step of blood clotting involves the activation of various clotting factors.
- These factors help in the formation of thrombin.
- Thrombin changes fibrinogen into fibrin.
- Fibrin forms a mesh.
- Platelets stick together and then attach to this fibrin mesh to form the clot.
The consequences can be severe if a clot forms in an undamaged blood vessel. This is when blood thinners become important. These medications interfere with aspects of the blood clotting process, such as clotting factors or platelets.
Types of Blood Thinners
Blood thinners work in different ways to prevent clots from being made. In some cases, they can stop pre-existing clots from growing bigger. Blood thinners are of two types: Anticoagulants and Antiplatelets.
Anticoagulants
Anticoagulants are blood thinning medications that negatively affect blood clotting factors. Some examples of anticoagulants are given below.
- Warfarin: blocks vitamin K, which is vital for forming clots.
- Dabigatran and edoxaban: block a protein molecule essential for clot formation.
- Heparin: is administered intravenously; it stops coagulation factors from activating.
Antiplatelets
Antiplatelets work by either directly stopping platelets from binding together or negatively affecting the signaling pathways that recruit platelets during clot formation.
Examples of antiplatelets are given below.
- Dipyridamole: This medicine impacts a molecule called cAMP, an important signaling molecule involved in blood coagulation.
- Abciximab: Attaches to platelets to stop them from sticking together.
- Aspirin: Stops platelets from coming together to produce a clot and also works as an anti-inflammatory.
Why and When Blood Thinners are Prescribed or Used
Blood thinners are used to treat many different conditions. Some disorders where blood thinners are routinely prescribed are listed below.
- Congenital heart defects: congenital heart disease increases the chance of clots forming.
- Atrial fibrillation: clots can form when the top two chambers, the atria, contract too fast and in an irregular rhythm.
- Heart valve replacement: if a heart valve is replaced surgically through open heart surgery or TAVR, blood thinners must be taken to prevent clot formation.
- Heart failure patients: patients with heart failure can easily produce clots, so blood thinners may sometimes be prescribed.
- Coronary artery disease: studies have shown a higher risk of emboli in patients with coronary artery disease.
- Deep vein thrombosis (DVT): occurs when a clot forms in a deep vein in one of the legs.
- Pulmonary embolism (PE): occurs when a clot has traveled to the lungs.
- Risk of clots post-surgery: surgery can lead to complications, including unusual clot formation.
- During dialysis: Dialysis involves using a machine to clean your blood; in order to do this properly, clots must be prevented from forming.
- During blood transfusions: clots need to be prevented from forming in blood that is to be used for transfusions.
The Benefits of Blood Thinners
Blood thinners prevent blood clots from forming when they shouldn’t. Many heart attacks and strokes are caused by blood clots; anticoagulants or antiplatelets can help prevent these problems. Blood thinners can save lives but need to be carefully monitored by physicians.
It is important to understand that only your doctor can tell you if you need to be taking blood thinners.
The Disadvantages of Blood Thinners
There are some drawbacks to using blood thinners
The potential side effects include:
- Easy bruising
- Bleeding gums
- Bleeding nose
- Bleeding from the stomach
- Bleeding from the rectum
- Uncontrolled heavy hemorrhage
Heavy bleeding rarely occurs, but it is worth noting as a risk. Certain conditions and interactions with other medicines increase the risk of severe bleeding. These are described below.
- Having liver disease poses a problem because it impacts clotting factors and can result in severe bleeding.
- Having kidney disease can mean a greater chance of hemorrhage.
- Drinking alcohol can increase the odds of an uncontrolled bleeding event if you are on blood thinners.
- Taking nonsteroidal anti-inflammatory medication, such as ibuprofen, along with blood thinners can also be dangerous, increasing the chances of internal bleeding.
Preventing Problems While on Blood Thinners
There are ways you can lessen or prevent some of the side effects. These are listed below.
- Avoid falls by wearing non-skid shoes.
- Do not walk around barefoot.
- Be very careful using any sharp objects like knives or scissors that could cut you.
- Do not start a new medication without consulting a doctor.
Signs that Blood Thinners are Causing Problems
Seek medical attention if you are on blood thinners and have any of the following symptoms:
- Vomit that is bright red or brown in color
- Red-colored or black tar-like stool
- Severe pain in the stomach
- Severe headache
- Blood in the urine
- Bruising that is unusual and frequent
Blood Thinners in Pregnancy
Blood thinner medication such as anticoagulants may pose a problem for pregnant women. While it could pose a risk to the fetus, not taking blood thinner medication can be risky for the mother if she has certain medical problems. Certain anticoagulants and antiplatelets may be dangerous depending on the particular situation.
This is why the best strategy for a pregnant woman is to consult her obstetrician regarding all medicines, including blood thinners, that she usually takes. Only a qualified doctor can decide which blood thinners a pregnant woman can safely take.
Conclusion
Blood thinners are medications that inhibit clots from being formed in the blood. These medicines are essential and most often used by people with certain medical conditions related to the heart and blood vessels. However, blood thinners can have dangerous side effects. It is crucial to always check with your doctor if you are taking blood thinners and experiencing unusual or unpleasant side effects.
To search for the best Cardiology healthcare providers in Croatia, Germany, India, Malaysia, Poland, Singapore, Spain, Thailand, Turkey, the UAE, the UK and The USA, please use the Mya Care Search engine

Dr. Rae Osborn has a Ph.D. in Biology from the University of Texas at Arlington. She was a tenured Associate Professor of Biology at Northwestern State University, where she taught many courses to Pre-nursing and Pre-medical students. She has written extensively on medical conditions and healthy lifestyle topics, including nutrition. She is from South Africa but lived and taught in the United States for 18 years.
Sources:
Featured Blogs

Medically Induced Coma: What It Is, How It Works, Who Benefits, and Recovery Outcomes


