Itchy and Painful: Herpes Zoster (Shingles)

What is Shingles?
Shingles, also known as herpes zoster, is a viral infection that is characterized by painful rashes appearing on one side of the face or body. Although not a life-threatening condition, it can cause some complications. The CDC reports that around one million cases of herpes zoster occur annually in the United States i.e., an incidence of about 4 in 1000. Among those aged 60 plus, the incidence goes up to 1 in 100.
What causes Shingles?
Shingles is caused by the reactivated varicella-zoster virus (VZV), which also causes chickenpox. After having chickenpox, the VZV lies dormant in the nervous system. Once it reactivates, it travels along nerve pathways to the skin, thus causing the classic painful, unilateral shingles rash. All patients with shingles have already had chickenpox, but not all patients with chickenpox will have shingles. Shingles can recur, but the majority of those affected usually only have one episode during their lifetime.
Who can get Shingles?
It is still unclear as to what triggers the reactivation of the varicella-zoster virus, but there are some risk factors that could increase the chance of developing shingles:
- Age older than 50 – age is a major risk factor for shingles. The risk increases with age.
- Immunocompromised individuals – those with comorbidities that can weaken the immune system, such as cancer, HIV, and solid organ transplants, have a higher risk of getting infected with VZV.
- Chemotherapy or radiation therapy – weakens the immune system and, therefore, increases the risk for infection.
- Certain medications – medications such as drugs given after organ transplants and prolonged use of systemic steroids can lower your resistance and impair the immune system.
- Trauma, stress
Recurrence is also higher in immunocompromised patients.
What are the symptoms of Shingles?
Rash
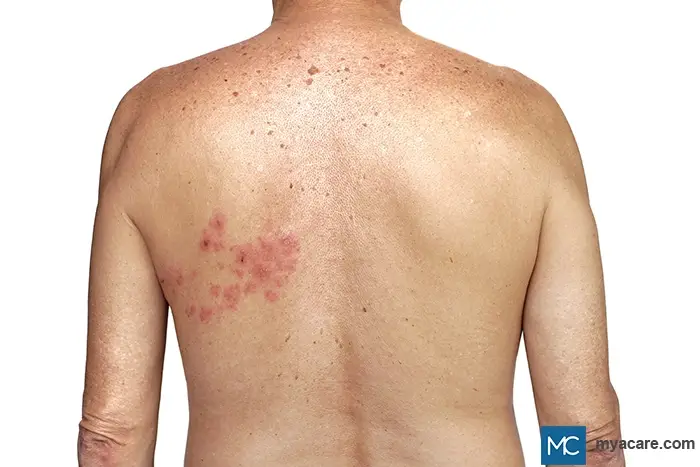
The rash usually affects only a section of one side of the face or body. Lesions are initially red, flat, or raised, with the appearance of fluid-filled small blisters (vesicles) within 12 to 24 hours. These blisters tend to form in groups and can continue to increase in number for up to 4 days. By the third day, there may be some lesions with pus or purulent discharge. The lesions will dry and develop crusts in 7 to 10 days. Crusting will usually persist for around 2-3 weeks.
Pain
Pain is the main symptom of shingles, most especially in the elderly. It usually precedes the appearance of rashes by 1-3 days. The pain can be described as tingling, burning, or even severe, deep, or lancinating pain. Other early symptoms may include fever, headache, chills, body weakness, and sensitivity to light.
Ophthalmic herpes zoster
VZV affecting the eye is called ophthalmic zoster. This can happen in about 10-15% of cases. Aside from the pain and blistering rash, patients can present with conjunctivitis, impaired corneal sensation, and corneal ulcerations. A referral to an Ophthalmologist may be warranted.
Is Shingles contagious?
The varicella-zoster virus is contagious. It can be passed through direct skin contact or through contact with the fluid or discharge of the open sores. The shingles virus, when passed on, cannot cause shingles; but can cause chickenpox, especially if the infected person doesn’t have a previous history of chickenpox or has never received the chickenpox vaccine. It is better to isolate, keep your rash covered, and avoid physical contact until the lesions are dry and crusted. Lesions that are dry and crusted are no longer contagious.
Should I see a doctor?
The diagnosis of shingles is fairly straightforward. However, approximately 1% to 4% of patients with shingles may get hospitalized due to complications. A visit to the doctor may be needed if:
- The patient is elderly
- The patient is immunocompromised
- The rash is widespread and severely painful
- The rash and pain occur near an eye
Diagnostic laboratory tests that may be performed involve using scrapings or a swab of the blister fluid sent to the laboratory for further examination.
What are the complications of Shingles?
Complications that may be seen in shingles include:
- Concomitant bacterial infections – especially if blisters are not properly treated
- Pneumonia – very rare
- Vision loss – from ophthalmic zoster
- Neurological problems – such as any numbness, itching, facial paralysis, or hearing problems
- Postherpetic neuralgia – most common complication
Postherpetic Neuralgia
The most common and most debilitating complication is called postherpetic neuralgia (PHN). This refers to the long-term nerve pain in the areas affected by the shingles rash. This can happen in around 10-18% of shingles patients, with an increased risk in the elderly. PHN can last for months or years.
How is Shingles treated?
While shingles has no cure, but early detection and treatment can hasten recovery and prevent complications.
The treatment options for shingles include:
- Antiviral medications – limit the extent, duration, and severity of pain and rashes. These oral medications work better if given within 72 hours of the start of symptoms. Medications include acyclovir, famciclovir, and valacyclovir. In immunocompromised patients, intravenous (IV) antivirals may be given.
- Pain medications/ Analgesics – helps relieve pain.
- Antibacterial medications – for cases with secondary bacterial infections.
Some home remedies and lifestyle modifications may include:
- Applying cool, wet compresses to help relieve itching and pain
- Taking cool baths
- Calamine lotion
- Reducing the amount of stress
- Covering the rash to prevent the spread
- Avoiding touching or scratching the rashes
- Avoiding direct contact with other people until crusting of rashes is observed
- Proper handwashing
Should I get the vaccine to prevent Shingles?
Vaccines for shingles and varicella-zoster virus are available and can help prevent or reduce the severity of the disease. Vaccines can also decrease the risk for complications such as postherpetic neuralgia. The recombinant zoster vaccine is recommended for adults 50 years and older, as well as for immunocompromised patients. Vaccines also have side effects and contraindications; therefore, it is better to discuss the options with your doctor to determine which vaccine is right for you.
To search for the best health providers for dermatology in Croatia, Germany, Greece, Italy, Malaysia, Singapore, Slovakia Spain, Thailand, The UAE, the UK, and the US, please use our free search engine.
To search for the best healthcare providers worldwide, please use the Mya Care search engine.
Dr. Lauren Livelo is a board-certified dermatologist from the Philippines. She has a degree in Medicine from the University of the East Ramon Magsaysay Memorial Medical Center, and has completed her dermatology residency training in the Research Institute for Tropical Medicine. Aside from her private practice, she enjoys writing about skin care and diseases of the skin.
References:
Featured Blogs

Medically Induced Coma: What It Is, How It Works, Who Benefits, and Recovery Outcomes


