What Is Hansen’s Disease (Leprosy)?
Hansen’s Disease, otherwise known as Leprosy, is an infection caused by the bacteria Mycobacterium leprae (M. leprae). The disease predominantly affects the skin, peripheral nerves, nasal mucosa, and the eyes. It targets the Schwann cells, which help regulate the function of the peripheral nervous system. M. leprae is a bacterium that multiplies very slowly, thus, it takes years of constant exposure to develop signs and symptoms of the infection. It can affect anyone at any age.
The number of cases of Hansen’s Disease is gradually decreasing, however, there still are areas in the world where Hansen’s Disease is endemic. This includes the following countries: Bangladesh, Philippines, Indonesia, India, Nepal, Myanmar, Sri Lanka, Brazil, Democratic Republic of Congo, Mozambique, Nigeria, Madagascar, Ethiopia, and the United Republic of Tanzania.
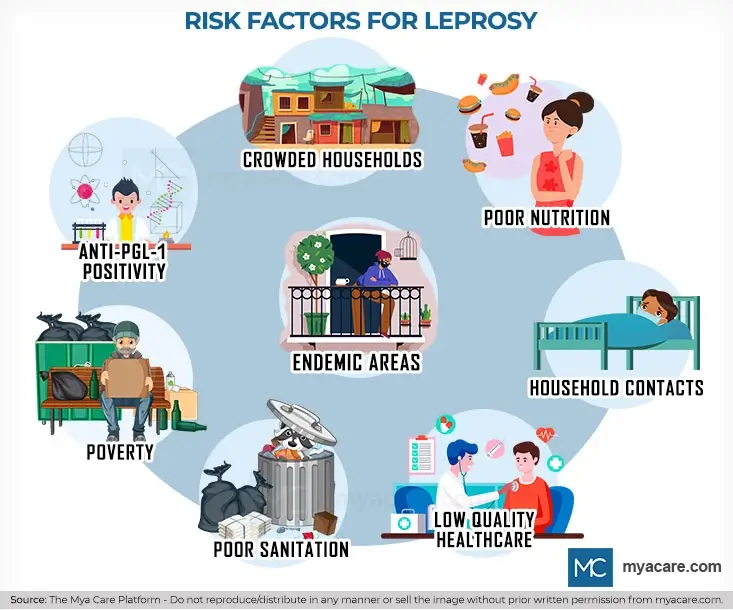
Risk Factors
- Household contacts of those with an untreated leprosy index case
- Having a positive anti-PGL-I titer denotes an 8-fold higher risk
- Living in an endemic area for leprosy
- Poverty
- Living in crowded households
- Poor nutritional status
- Poor sanitation
- Lack of proper health care availability
Leprosy is not transmissible through casual contact such as shaking hands, hugging, or sitting next to an infected person. Exposure and close contact with an untreated case for extended periods of time is required to catch the disease. In addition, more than 90% of the population worldwide has a natural immunity to the disease; therefore, the overall risk of getting Hansen’s disease is quite low.
What are the Symptoms of Hansen’s Disease?
CUTANEOUS FINDINGS
- Hypopigmented, hyperpigmented, or red patches or plaques on the skin that have impaired sensation or loss of sensation and make no sweat
- Nodules or lumps on the face, earlobes, or any part of the skin
- Leonine facies
- Hair loss on the eyebrows or eyelashes (madarosis)
- Dry skin
NON-CUTANEOUS FINDINGS
- Muscle weakness or paralysis
- Nerve enlargement
- Eye problems
How is it Diagnosed?
Taking a sample of the affected skin by performing a skin biopsy and looking at the specimen through a microscope can help in the diagnosis of Hansen’s Disease. Slit skin smears from the earlobes, elbows, or knees can help determine the number of acid-fast bacilli detected from the skin sample, and is essential in determining the spectrum of the disease. Other diagnostics that may be useful include a nerve biopsy if thickened nerves are present, as well as nerve conduction studies to evaluate neuropathy.
What is the Treatment for Hansen’s Disease?
The treatment for Hansen’s Disease usually involves the use of a multi-drug regimen composed of three (3) antibiotics namely: rifampicin, dapsone, and clofazimine. It is better to consult with your physician regarding the treatment regimen, as there are specific instructions on how the medications are taken, as well as how long one should take them. Steroids and thalidomide have anti-inflammatory uses which can help manage leprosy reactions. Analgesics may also be given to address the neuropathic pain.
Complications of Hansen’s Disease
- Disfigurement and deformity, most commonly in the hands and feet (claw hand, foot drop)
- Loss of corneal sensation in the eyes, along with possible blindness, lagophthalmos, weakening of the peripheral muscles
- Saddle-nose deformity
- Muscle atrophy
Prevention
The initial step of prevention is to do a contact examination. It is better to screen the household members of those afflicted with leprosy, as well as those contacts who are in close proximity with the patient. Rifampicin is generally given to prevent infection, and the Bacillus Calmette-Guerin (BCG) vaccination is also given for immunoprophylaxis.
Clinical Course and Prognosis
Hansen’s Disease is treatable, especially if caught early. Some problems that can arise include leprosy reactions, which are episodes of inflammation that can involve the skin and/or nerves. Constant follow-up with your physician is needed. Leprosy patients also face a lot of discrimination from society. Counseling and support groups may be avenues that can help patients who have this disease. People who have leprosy can lead a normal and active life during and after treatment.
To search for the best health providers for dermatology in Croatia, Germany, Greece, Italy, Malaysia, Singapore, Slovakia Spain, Thailand, The UAE, the UK, and the US, please use our free search engine.
To search for the best healthcare providers worldwide, please use the Mya Care search engine.
Dr. Lauren Livelo is a board-certified dermatologist from the Philippines. She has a degree in Medicine from the University of the East Ramon Magsaysay Memorial Medical Center, and has completed her dermatology residency training in the Research Institute for Tropical Medicine. Aside from her private practice, she enjoys writing about skin care and diseases of the skin.
References:
Featured Blogs



