What Is Hidradenitis Suppurativa?

Hidradenitis suppurativa (HS), also called acne inversa, is a chronic inflammatory skin disorder which affects the hair follicles in the intertriginous and genital areas of the body. Lesions usually appear as persistent or recurrent pimples and boils, which can worsen to form lumps, cysts, and abscesses, as well as scars and pus-filled tunnels on the axillae, groin, inner thighs, or below the breasts.
What is the Cause of Hidradenitis Suppurativa?
The cause of HS is still unclear, but it seems to be due to a combination of factors, such as genetics, hormonal dysregulation, environmental factors, and immune dysregulation. HS affects areas of the body with apocrine and sebaceous glands. There is occlusion of the hair follicles with keratin, sebum, sweat, and bacteria, which can cause inflammation, leading to the formation of painful pimple-like lesions which can evolve into cysts and abscesses filled with pus.
Who Can Get Hidradenitis Suppurativa?
Women have a higher risk of developing HS compared to men. Most patients develop HS between puberty to age 40. Risk factors include:
- Genetics (family history)
- Obesity and the metabolic syndrome
- Smoking – can be a trigger for HS
- African ethnicity – African Americans tend to have a greater risk of developing more severe HS
- Associated diseases: inflammatory bowel disease, follicular occlusion syndrome, PASH syndrome (pyoderma gangrenosum, acne, suppurative hidradenitis), PAPASH syndrome (pyogenic arthritis, pyoderma gangrenosum, acne, suppurative hidradenitis), and other skin diseases such as psoriasis and acne
What are the Signs and Symptoms?
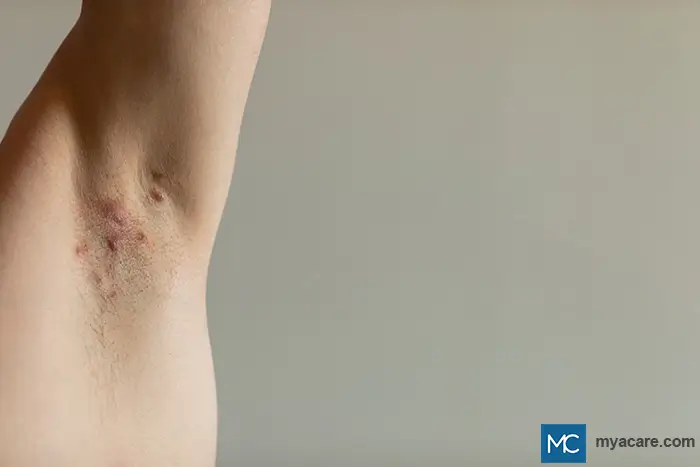
HS lesions usually affect the armpits, neck, inframammary areas, and inner thighs. It can also involve the anogenital area, such as the mons pubis, vulva, scrotum, and buttocks. Lesions can initially appear as tender papules or nodules that can grow and coalesce, and evolve into large, painful abscesses that contain foul-smelling purulent material. Lesions can involute in 7 to 10 days, but some lesions heal very slowly. HS lesions tend to be recurrent, and these reappearances and repetitive healing can lead to sinus tract formation and deeply scarred skin or rope-like bands.
How is it Diagnosed?
Hidradenitis suppurativa is usually diagnosed through clinical history and physical examination. There is no existing confirmatory test for HS. There is, however, a diagnostic criterion wherein all three components should be satisfied in order to arrive at a definite diagnosis. It includes:
- Presence of characteristic lesions (1 or more): painful nodules, abscesses, draining sinuses, bridged scars
- Lesions must exhibit the typical distribution: axillae, groin, buttocks, inframammary region, perineal area
- History of chronicity and recurrence of symptoms
There is also a criteria for the severity of lesions, called the Hurley staging. Most patients have stage I disease.
- Hurley Stage I: having recurrent abscesses without scarring or sinus tract formation
- Hurley Stage II: having recurrent abscesses with scarring and sinus tract formation separated by normal skin
- Hurley Stage III: having recurrent abscesses, diffuse scarring, and interconnecting sinus tracts with minimal to no normal skin between lesions
What are the Treatment Options for Hidradenitis Suppurativa?
There are various treatment options for HS, however, none of them offer a complete cure for the disease. Treatment is done with the goal of reducing the impact of the disease, treating any infection, relieving pain, and improving the quality of life. Some of the treatment and management options for mild to moderate disease include the following:
- Oral antibiotics like clindamycin, doxycycline, rifampin, and dapsone
- Hormonal therapies such as oral contraceptives, finasteride, spironolactone, and metformin
- Alternative medicine, including oral vitamin D, oral zinc, and magnesium sulfate salt baths
- Procedures such as deroofing (either surgical or with the use of a CO2 laser), intralesional steroids, incision and drainage, local excision, and the use of an Nd:YAG laser
Management options for moderate to severe cases include the following:
- Biologics like adalimumab (the only FDA-approved biologic for HS)
- Systemic antibiotics such as ertapenem
- Systemic immunosuppressants and immunomodulators like apremilast, colchicine, and systemic steroids
- Retinoids such as acitretin and isotretinoin
- Procedures including CO2 laser excision, wide surgical excision, and deroofing
Lifestyle modifications and other possible measures to treat patients with HS include:
- Cessation of smoking
- Weight loss
- Wearing loose-fitting clothing
- Analgesics for pain
- Managing anxiety and stress
What is the Prognosis for Hidradenitis Suppurativa?
There is no cure for hidradenitis suppurativa, but it can be managed to lessen the symptoms. Many patients can experience limited mobility due to the formation of fibrosis and dermal contractures secondary to the scarring brought about by HS. There can be spontaneous improvement of lesions, but the scarring will remain.
Take-Home Messages
Hidradenitis suppurativa is a chronic skin disease that affects the apocrine and sebaceous glands. Patients with hidradenitis suppurativa experience a decrease in quality of life, as the disease affects their activities of daily living, social functioning, and psychological health. It is better to see a dermatologist in order to have a guided treatment plan. A referral to other specialties such as surgery, psychiatry (for feelings of depression and anxiety), or internal medicine may be warranted for more complicated cases.
To search for the best health providers for dermatology in Croatia, Germany, Greece, Italy, Malaysia, Singapore, Slovakia, Spain, Thailand, The UAE, the UK, and the US, please use our free search engine.
To search for the best healthcare providers worldwide, please use the Mya Care search engine.
Dr. Lauren Livelo is a board-certified dermatologist from the Philippines. She has a degree in Medicine from the University of the East Ramon Magsaysay Memorial Medical Center, and has completed her dermatology residency training in the Research Institute for Tropical Medicine. Aside from her private practice, she enjoys writing about skin care and diseases of the skin.
References:
Featured Blogs

Medically Induced Coma: What It Is, How It Works, Who Benefits, and Recovery Outcomes


